El accidente cerebrovascular (también conocido como accidente cerebrovascular ( ACV ) o ataque cerebral ) es una afección médica en la que un flujo sanguíneo deficiente al cerebro provoca la muerte celular . [5] Hay dos tipos principales de accidente cerebrovascular:
Ambos provocan que partes del cerebro dejen de funcionar correctamente. [5]
Los signos y síntomas de un accidente cerebrovascular pueden incluir incapacidad para moverse o sentir en un lado del cuerpo, problemas para comprender o hablar , mareos o pérdida de la visión en un lado . [2] [3] Los signos y síntomas suelen aparecer poco después de que se haya producido el accidente cerebrovascular. [3] Si los síntomas duran menos de una o dos horas, el accidente cerebrovascular es un ataque isquémico transitorio (AIT), también llamado miniaccidente cerebrovascular. [3] El accidente cerebrovascular hemorrágico también puede estar asociado con un dolor de cabeza intenso . [3] Los síntomas del accidente cerebrovascular pueden ser permanentes. [5] Las complicaciones a largo plazo pueden incluir neumonía y pérdida del control de la vejiga . [3]
El mayor factor de riesgo para el accidente cerebrovascular es la presión arterial alta . [7] Otros factores de riesgo incluyen colesterol alto en sangre , tabaquismo , obesidad , diabetes mellitus , un AIT previo, enfermedad renal terminal y fibrilación auricular . [2] [7] [8] El accidente cerebrovascular isquémico generalmente es causado por el bloqueo de un vaso sanguíneo, aunque también hay causas menos comunes. [13] [14] [15] El accidente cerebrovascular hemorrágico es causado por sangrado directamente en el cerebro o en el espacio entre las membranas del cerebro . [13] [16] El sangrado puede ocurrir debido a un aneurisma cerebral roto . [13] El diagnóstico generalmente se basa en un examen físico y está respaldado por imágenes médicas como una tomografía computarizada o una resonancia magnética . [9] Una tomografía computarizada puede descartar sangrado, pero no necesariamente descartar isquemia, que al principio generalmente no aparece en una tomografía computarizada. [10] Se realizan otras pruebas, como un electrocardiograma (ECG) y análisis de sangre, para determinar los factores de riesgo y descartar otras posibles causas. [9] Un nivel bajo de azúcar en sangre puede provocar síntomas similares. [9]
La prevención incluye la disminución de los factores de riesgo, la cirugía para abrir las arterias del cerebro en aquellos con estrechamiento carotídeo problemático y warfarina en personas con fibrilación auricular . [2] Los médicos pueden recomendar aspirina o estatinas para la prevención. [2] El accidente cerebrovascular es una emergencia médica. [5] Los accidentes cerebrovasculares isquémicos, si se detectan dentro de las tres a cuatro horas y media, pueden tratarse con medicamentos que pueden descomponer el coágulo , [2] mientras que los accidentes cerebrovasculares hemorrágicos a veces se benefician de la cirugía . [2] El tratamiento para intentar recuperar la función perdida se llama rehabilitación del accidente cerebrovascular , e idealmente se lleva a cabo en una unidad de accidentes cerebrovasculares; sin embargo, estas no están disponibles en gran parte del mundo. [2]
En 2023, 15 millones de personas en todo el mundo sufrieron un accidente cerebrovascular. [17] En 2021, el accidente cerebrovascular fue la tercera causa más importante de muerte, responsable de aproximadamente el 10% del total de muertes. [18] En 2015, hubo alrededor de 42,4 millones de personas que habían tenido un accidente cerebrovascular previamente y todavía estaban vivas. [11] Entre 1990 y 2010, la incidencia anual de accidente cerebrovascular disminuyó aproximadamente un 10% en el mundo desarrollado , pero aumentó un 10% en el mundo en desarrollo. [19] En 2015, el accidente cerebrovascular fue la segunda causa más frecuente de muerte después de la enfermedad de las arterias coronarias , lo que representa 6,3 millones de muertes (11% del total). [12] Aproximadamente 3,0 millones de muertes resultaron de un accidente cerebrovascular isquémico, mientras que 3,3 millones de muertes resultaron de un accidente cerebrovascular hemorrágico. [12] Aproximadamente la mitad de las personas que han tenido un accidente cerebrovascular viven menos de un año. [2] En general, dos tercios de los casos de accidente cerebrovascular ocurrieron en personas mayores de 65 años. [19]
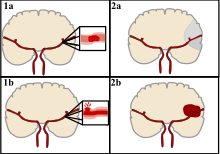

El accidente cerebrovascular se puede clasificar en dos categorías principales: isquémico y hemorrágico . [20] El accidente cerebrovascular isquémico es causado por la interrupción del suministro de sangre al cerebro, mientras que el accidente cerebrovascular hemorrágico resulta de la ruptura de un vaso sanguíneo o una estructura vascular anormal .
Aproximadamente el 87 % de los accidentes cerebrovasculares son isquémicos y el resto son hemorrágicos. Se pueden producir hemorragias en áreas de isquemia, una afección conocida como " transformación hemorrágica ". Se desconoce cuántos casos de accidente cerebrovascular hemorrágico comienzan en realidad como accidente cerebrovascular isquémico. [2]
En la década de 1970, la Organización Mundial de la Salud definió el "accidente cerebrovascular" como un "déficit neurológico de causa cerebrovascular que persiste más allá de 24 horas o se interrumpe por la muerte dentro de las 24 horas", [21] aunque la palabra "accidente cerebrovascular" tiene siglos de antigüedad. Se suponía que esta definición reflejaba la reversibilidad del daño tisular y se ideó para ese propósito, y el marco de tiempo de 24 horas se eligió arbitrariamente. El límite de 24 horas separa el accidente cerebrovascular del ataque isquémico transitorio , que es un síndrome relacionado con los síntomas del accidente cerebrovascular que se resuelven completamente en 24 horas. [2] Con la disponibilidad de tratamientos que pueden reducir la gravedad del accidente cerebrovascular cuando se administran de manera temprana, muchos prefieren ahora una terminología alternativa, como "ataque cerebral" y "síndrome cerebrovascular isquémico agudo" (modelado a partir del ataque cardíaco y el síndrome coronario agudo , respectivamente), para reflejar la urgencia de los síntomas del accidente cerebrovascular y la necesidad de actuar rápidamente. [22]
Durante un accidente cerebrovascular isquémico, el suministro de sangre a una parte del cerebro disminuye, lo que provoca una disfunción del tejido cerebral en esa zona. Existen cuatro razones por las que esto puede suceder:
El accidente cerebrovascular sin una explicación obvia se denomina accidente cerebrovascular criptogénico ( idiopático ) y constituye el 30-40% de todos los casos de accidente cerebrovascular isquémico. [2] [25]
Existen sistemas de clasificación para el ictus isquémico agudo. La clasificación del Oxford Community Stroke Project (OCSP, también conocida como clasificación de Bamford u Oxford) se basa principalmente en los síntomas iniciales; según la extensión de los síntomas, el episodio de ictus se clasifica como infarto total de la circulación anterior (TACI), infarto parcial de la circulación anterior (PACI), infarto lacunar (LACI) o infarto de la circulación posterior (POCI). Estas cuatro entidades predicen la extensión del ictus, el área del cerebro afectada, la causa subyacente y el pronóstico. [26] [27]
La clasificación TOAST (Trial of Org 10172 in Acute Stroke Treatment) se basa en los síntomas clínicos, así como en los resultados de investigaciones posteriores; sobre esta base, el accidente cerebrovascular se clasifica como debido a
(1) trombosis o embolia debida a aterosclerosis de una arteria grande,
(2) una embolia que se origina en el corazón ,
(3) bloqueo completo de un vaso sanguíneo pequeño,
(4) otra causa determinada,
(5) causa indeterminada (dos causas posibles, ninguna causa identificada o investigación incompleta). [28]
Los consumidores de estimulantes como la cocaína y la metanfetamina tienen un alto riesgo de sufrir un accidente cerebrovascular isquémico. [29]
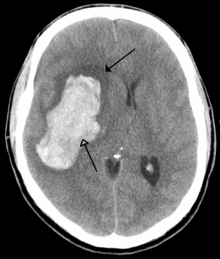
Existen dos tipos principales de accidente cerebrovascular hemorrágico: [30] [31]
Los dos tipos principales de accidente cerebrovascular hemorrágico mencionados anteriormente también son dos formas diferentes de hemorragia intracraneal , que es la acumulación de sangre en cualquier lugar dentro de la bóveda craneal ; pero las otras formas de hemorragia intracraneal, como el hematoma epidural (sangrado entre el cráneo y la duramadre , que es la capa gruesa más externa de las meninges que rodean el cerebro) y el hematoma subdural (sangrado en el espacio subdural ), no se consideran "accidente cerebrovascular hemorrágico". [32]
El accidente cerebrovascular hemorrágico puede ocurrir en el contexto de alteraciones de los vasos sanguíneos del cerebro, como la angiopatía amiloide cerebral , la malformación arteriovenosa cerebral y un aneurisma intracraneal , que pueden causar hemorragia intraparenquimatosa o subaracnoidea. [33]
Además del deterioro neurológico, el accidente cerebrovascular hemorrágico suele provocar síntomas específicos (por ejemplo, la hemorragia subaracnoidea clásicamente causa un dolor de cabeza intenso conocido como dolor de cabeza en trueno ) o revelar evidencia de una lesión cerebral previa .
Los síntomas de un accidente cerebrovascular suelen comenzar de repente, en cuestión de segundos o minutos, y en la mayoría de los casos no progresan más. Los síntomas dependen de la zona del cerebro afectada. Cuanto más extensa sea la zona del cerebro afectada, más funciones es probable que se pierdan. Algunas formas de accidente cerebrovascular pueden causar síntomas adicionales. Por ejemplo, en la hemorragia intracraneal, la zona afectada puede comprimir otras estructuras. La mayoría de las formas de accidente cerebrovascular no se asocian con dolor de cabeza , aparte de la hemorragia subaracnoidea y la trombosis venosa cerebral y, ocasionalmente, la hemorragia intracerebral. [33]

Se han propuesto sistemas para aumentar el reconocimiento del ACV. La debilidad facial de aparición repentina, la desviación de los brazos (es decir, si una persona, cuando se le pide que levante ambos brazos, involuntariamente deja que uno de ellos se desplace hacia abajo) y el habla anormal son los hallazgos que tienen más probabilidades de llevar a la identificación correcta de un caso de ACV, lo que aumenta la probabilidad en 5,5 cuando al menos uno de estos está presente. De manera similar, cuando los tres están ausentes, la probabilidad de ACV disminuye ( razón de probabilidad de -0,39). [34] Si bien estos hallazgos no son perfectos para diagnosticar el ACV, el hecho de que se puedan evaluar con relativa rapidez y facilidad los hace muy valiosos en el contexto agudo.
Un mnemónico para recordar los signos de advertencia de un accidente cerebrovascular es FAST (facial droop, arm weakness, speech difficulty, and time to call emergency services), [35] tal como lo recomiendan el Departamento de Salud (Reino Unido) y la Stroke Association , la American Stroke Association y la National Stroke Association (EE. UU.). FAST es menos confiable en el reconocimiento de un accidente cerebrovascular de circulación posterior. [36] El mnemónico revisado BE FAST , que agrega equilibrio (dificultad repentina para mantener el equilibrio al caminar o estar de pie) y vista (nueva aparición de visión borrosa o doble o pérdida repentina e indolora de la vista) a la evaluación, se ha propuesto para abordar esta deficiencia y mejorar aún más la detección temprana del accidente cerebrovascular. [37] [38] Otras escalas para la detección prehospitalaria del accidente cerebrovascular incluyen la Escala de detección de accidentes cerebrovasculares prehospitalarios de Los Ángeles (LAPSS) [39] y la Escala de accidentes cerebrovasculares prehospitalarios de Cincinnati (CPSS), [40] en las que se basó el método FAST. [41] El uso de estas escalas está recomendado por las pautas profesionales. [42]
En el caso de las personas derivadas a urgencias , se considera importante el reconocimiento temprano del ictus, ya que esto puede agilizar las pruebas de diagnóstico y los tratamientos. Para este fin, se recomienda un sistema de puntuación denominado ROSIER (reconocimiento del ictus en urgencias), que se basa en características de la historia clínica y el examen físico. [42] [43]
La pérdida de conciencia , el dolor de cabeza y los vómitos suelen ocurrir con mayor frecuencia en el accidente cerebrovascular hemorrágico que en la trombosis debido al aumento de la presión intracraneal por la fuga de sangre que comprime el cerebro.
Si los síntomas son máximos al inicio, es más probable que la causa sea una hemorragia subaracnoidea o un accidente cerebrovascular embólico.
Si el área del cerebro afectada incluye una de las tres vías principales del sistema nervioso central (el tracto espinotalámico , el tracto corticoespinal y la vía de la columna dorsal-lemnisco medial) , los síntomas pueden incluir:
En la mayoría de los casos, los síntomas afectan sólo a un lado del cuerpo (unilateral). El defecto en el cerebro suele estar en el lado opuesto del cuerpo. Sin embargo, dado que estas vías también recorren la médula espinal y cualquier lesión allí también puede producir estos síntomas, la presencia de cualquiera de ellos no indica necesariamente un accidente cerebrovascular. Además de las vías del sistema nervioso central mencionadas anteriormente, el tronco encefálico da origen a la mayoría de los doce nervios craneales . Por lo tanto, un accidente cerebrovascular del tronco encefálico que afecte al tronco encefálico y al cerebro puede producir síntomas relacionados con déficits en estos nervios craneales: [ cita requerida ]
Si está afectada la corteza cerebral , las vías del sistema nervioso central pueden verse afectadas nuevamente, pero también pueden producirse los siguientes síntomas:
Si está afectado el cerebelo , puede haber ataxia , que incluye:
En los días previos a un ictus (generalmente en los 7 días previos, incluso el anterior), una proporción considerable de pacientes presentan un “cefalea centinela”: un dolor de cabeza intenso e inusual que indica un problema. [45] Su aparición hace aconsejable buscar revisión médica y considerar la prevención contra el ictus.
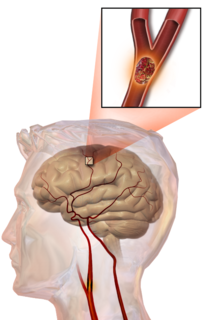
En el ictus trombótico, un trombo [46] (coágulo sanguíneo) suele formarse alrededor de las placas ateroscleróticas . Dado que el bloqueo de la arteria es gradual, la aparición del ictus trombótico sintomático es más lenta que la del ictus hemorrágico. Un trombo en sí mismo (incluso si no bloquea completamente el vaso sanguíneo) puede provocar un ictus embólico (ver más abajo) si el trombo se desprende y viaja por el torrente sanguíneo, momento en el que se denomina émbolo . Dos tipos de trombosis pueden causar un ictus:
La anemia provoca un aumento del flujo sanguíneo en el sistema circulatorio. Esto hace que las células endoteliales de los vasos sanguíneos expresen factores de adhesión que favorecen la coagulación de la sangre y la formación de trombos. [51] La anemia falciforme , que puede provocar que las células sanguíneas se aglomeren y bloqueen los vasos sanguíneos, también puede provocar un accidente cerebrovascular. El accidente cerebrovascular es la segunda causa principal de muerte en personas menores de 20 años con anemia falciforme. [52] La contaminación del aire también puede aumentar el riesgo de accidente cerebrovascular. [53]
Un accidente cerebrovascular embólico se refiere a una embolia arterial (un bloqueo de una arteria) causada por un émbolo , una partícula o residuo que viaja en el torrente sanguíneo arterial y que se origina en otro lugar. Un émbolo es con mayor frecuencia un trombo, pero también puede ser una serie de otras sustancias, como grasa (p. ej., de la médula ósea en un hueso roto ), aire, células cancerosas o grupos de bacterias (generalmente de endocarditis infecciosa ). [54]
Dado que el émbolo se origina en otra parte, la terapia local resuelve el problema solo temporalmente. Por lo tanto, se debe identificar la fuente del émbolo. Debido a que el bloqueo embólico comienza de manera repentina, los síntomas suelen ser máximos al principio. Además, los síntomas pueden ser transitorios a medida que el émbolo se reabsorbe parcialmente y se desplaza a una ubicación diferente o se disipa por completo.
Los émbolos se originan con mayor frecuencia en el corazón (especialmente en la fibrilación auricular ), pero pueden originarse en otras partes del árbol arterial. En la embolia paradójica , una trombosis venosa profunda embola a través de un defecto septal auricular o ventricular en el corazón hacia el cerebro. [54]
Las causas de accidente cerebrovascular relacionadas con el corazón se pueden distinguir entre riesgo alto y riesgo bajo: [55]
Entre aquellos que tienen un bloqueo completo de una de las arterias carótidas, el riesgo de sufrir un accidente cerebrovascular en ese lado es de aproximadamente un uno por ciento al año. [56]
Una forma especial de accidente cerebrovascular embólico es el accidente cerebrovascular embólico de origen indeterminado (ESUS). Este subconjunto del accidente cerebrovascular criptogénico se define como un infarto cerebral no lacunar sin estenosis arterial proximal ni fuentes cardioembólicas. Aproximadamente uno de cada seis casos de accidente cerebrovascular isquémico podría clasificarse como ESUS. [57]
La hipoperfusión cerebral es la reducción del flujo sanguíneo a todas las partes del cerebro. La reducción podría darse en una parte particular del cerebro dependiendo de la causa. Se debe más comúnmente a una insuficiencia cardíaca por paro cardíaco o arritmias , o por un gasto cardíaco reducido como resultado de un infarto de miocardio , embolia pulmonar , derrame pericárdico o hemorragia. [ cita requerida ] La hipoxemia (bajo contenido de oxígeno en la sangre) puede precipitar la hipoperfusión. Debido a que la reducción del flujo sanguíneo es global, todas las partes del cerebro pueden verse afectadas, especialmente las áreas vulnerables "de cuenca" (regiones de la zona fronteriza irrigadas por las arterias cerebrales principales). Un accidente cerebrovascular de cuenca se refiere a la afección en la que se ve comprometido el suministro de sangre a estas áreas. El flujo sanguíneo a estas áreas no necesariamente se detiene, sino que puede disminuir hasta el punto en que puede producirse daño cerebral.
La trombosis de los senos venosos cerebrales provoca un accidente cerebrovascular debido al aumento local de la presión venosa, que supera la presión generada por las arterias. Los infartos tienen más probabilidades de sufrir una transformación hemorrágica (fuga de sangre hacia la zona dañada) que otros tipos de accidente cerebrovascular isquémico. [24]
Generalmente ocurre en arterias pequeñas o arteriolas y comúnmente se debe a hipertensión, [58] malformaciones vasculares intracraneales (incluyendo angiomas cavernosos o malformaciones arteriovenosas ), angiopatía amiloide cerebral o infartos en los que se ha producido una hemorragia secundaria. [2] Otras causas potenciales son traumatismos, trastornos hemorrágicos , angiopatía amiloide , consumo de drogas ilícitas (p. ej., anfetaminas o cocaína ). El hematoma se agranda hasta que la presión del tejido circundante limita su crecimiento, o hasta que se descomprime vaciándose en el sistema ventricular , el LCR o la superficie pial. Un tercio del sangrado intracerebral se produce en los ventrículos del cerebro. La HIC tiene una tasa de mortalidad del 44 por ciento después de 30 días, más alta que el accidente cerebrovascular isquémico o la hemorragia subaracnoidea (que técnicamente también pueden clasificarse como un tipo de accidente cerebrovascular [2] ).
Otras causas pueden incluir el espasmo de una arteria. Esto puede ocurrir debido a la cocaína . [59] El cáncer también es otra causa potencial bien reconocida de accidente cerebrovascular. Aunque la malignidad en general puede aumentar el riesgo de accidente cerebrovascular, ciertos tipos de cáncer como el de páncreas, pulmón y estómago se asocian típicamente con un mayor riesgo de tromboembolia. Se cree que el mecanismo por el cual el cáncer aumenta el riesgo de accidente cerebrovascular es secundario a una hipercoagulabilidad adquirida . [60]
El accidente cerebrovascular silencioso es un accidente cerebrovascular que no presenta síntomas externos y, por lo general, las personas no saben que lo han sufrido. A pesar de no causar síntomas identificables, el accidente cerebrovascular silencioso aún daña el cerebro y coloca a la persona en mayor riesgo de sufrir un ataque isquémico transitorio y un accidente cerebrovascular mayor en el futuro. Por el contrario, quienes han tenido un accidente cerebrovascular importante también corren el riesgo de sufrir un accidente cerebrovascular silencioso. [61] En un amplio estudio realizado en 1998, se estimó que más de 11 millones de personas habían sufrido un accidente cerebrovascular en los Estados Unidos. Aproximadamente 770.000 de ellos fueron sintomáticos y 11 millones fueron los primeros infartos o hemorragias silenciosos detectados mediante resonancia magnética . El accidente cerebrovascular silencioso generalmente causa lesiones que se detectan mediante el uso de neuroimagen, como la resonancia magnética . Se estima que el accidente cerebrovascular silencioso ocurre a una tasa cinco veces mayor que el accidente cerebrovascular sintomático. [62] [63] El riesgo de accidente cerebrovascular silencioso aumenta con la edad, pero también puede afectar a adultos más jóvenes y niños, especialmente aquellos con anemia aguda . [62] [64]

El accidente cerebrovascular isquémico se produce debido a una pérdida de suministro de sangre a una parte del cerebro, lo que inicia la cascada isquémica . [65] La aterosclerosis puede interrumpir el suministro de sangre al estrechar el lumen de los vasos sanguíneos, lo que lleva a una reducción del flujo sanguíneo al causar la formación de coágulos de sangre dentro del vaso o al liberar lluvias de pequeños émbolos a través de la desintegración de las placas ateroscleróticas. [66] El infarto embólico ocurre cuando los émbolos formados en otra parte del sistema circulatorio, típicamente en el corazón como consecuencia de la fibrilación auricular, o en las arterias carótidas, se desprenden, ingresan a la circulación cerebral, luego se alojan y bloquean los vasos sanguíneos cerebrales. Dado que los vasos sanguíneos en el cerebro ahora están bloqueados, el cerebro pierde energía y, por lo tanto, recurre al uso del metabolismo anaeróbico dentro de la región del tejido cerebral afectada por la isquemia. El metabolismo anaeróbico produce menos trifosfato de adenosina (ATP) pero libera un subproducto llamado ácido láctico . El ácido láctico es un irritante que podría destruir células, ya que es un ácido y altera el equilibrio ácido-base normal en el cerebro. La zona de isquemia se denomina " penumbra isquémica ". [67] Después del evento isquémico inicial, la penumbra pasa de una remodelación tisular caracterizada por daño a una remodelación caracterizada por reparación. [68]
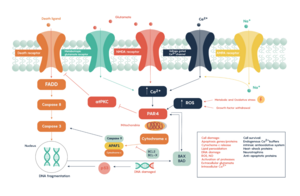
A medida que el oxígeno o la glucosa se agotan en el tejido cerebral isquémico, la producción de compuestos de fosfato de alta energía, como el trifosfato de adenosina (ATP), falla, lo que lleva al fracaso de los procesos dependientes de energía (como el bombeo de iones) necesarios para la supervivencia de las células del tejido. Esto desencadena una serie de eventos interrelacionados que resultan en daño celular y muerte. Una causa importante de daño neuronal es la liberación del neurotransmisor excitatorio glutamato. La concentración de glutamato fuera de las células del sistema nervioso normalmente se mantiene baja por los llamados transportadores de captación, que son alimentados por los gradientes de concentración de iones (principalmente Na + ) a través de la membrana celular. Sin embargo, el accidente cerebrovascular corta el suministro de oxígeno y glucosa que alimenta las bombas de iones que mantienen estos gradientes. Como resultado, los gradientes de iones transmembrana disminuyen y los transportadores de glutamato invierten su dirección, liberando glutamato en el espacio extracelular. El glutamato actúa sobre los receptores de las células nerviosas (especialmente los receptores NMDA), lo que produce un influjo de calcio que activa las enzimas que digieren las proteínas, los lípidos y el material nuclear de las células. El influjo de calcio también puede provocar la falla de las mitocondrias , lo que puede conducir a un mayor agotamiento de la energía y puede desencadenar la muerte celular debido a la muerte celular programada . [69]
La isquemia también induce la producción de radicales libres de oxígeno y otras especies reactivas de oxígeno . Estas reaccionan con una serie de elementos celulares y extracelulares y los dañan. Pueden producirse daños en el revestimiento de los vasos sanguíneos o en el endotelio. Estos procesos son los mismos para cualquier tipo de tejido isquémico y se denominan colectivamente cascada isquémica . Sin embargo, el tejido cerebral es especialmente vulnerable a la isquemia, ya que tiene poca reserva respiratoria y depende completamente del metabolismo aeróbico , a diferencia de la mayoría de los demás órganos.

El cerebro puede compensar el flujo sanguíneo inadecuado en una sola arteria mediante el sistema colateral. Este sistema se basa en la conexión eficiente entre las arterias carótida y vertebral a través del polígono de Willis y, en menor medida, las arterias principales que irrigan los hemisferios cerebrales . Sin embargo, las variaciones en el polígono de Willis, el calibre de los vasos colaterales y las lesiones arteriales adquiridas, como la aterosclerosis, pueden alterar este mecanismo compensatorio, aumentando el riesgo de isquemia cerebral resultante del bloqueo de la arteria. [70]
La magnitud del daño depende de la duración y la gravedad de la isquemia. Si la isquemia persiste durante más de 5 minutos con una perfusión inferior al 5% de lo normal, algunas neuronas morirán. Sin embargo, si la isquemia es leve, el daño se producirá lentamente y puede tardar hasta 6 horas en destruir por completo el tejido cerebral. En caso de isquemia grave que dure más de 15 a 30 minutos, todo el tejido afectado morirá, lo que provocará un infarto. La velocidad del daño se ve afectada por la temperatura, ya que la hipertermia acelera el daño y la hipotermia lo ralentiza, entre otros factores. La rápida restauración del flujo sanguíneo a los tejidos isquémicos puede reducir o revertir la lesión, especialmente si los tejidos aún no están dañados de forma irreversible. Esto es particularmente importante para las áreas moderadamente isquémicas (penumbras) que rodean las áreas de isquemia grave, que aún pueden salvarse gracias al flujo colateral. [70] [71] [72]
El accidente cerebrovascular hemorrágico se clasifica en función de su patología subyacente. Algunas causas de accidente cerebrovascular hemorrágico son hemorragia hipertensiva , aneurisma roto, fístula AV rota , transformación de infarto isquémico previo y sangrado inducido por fármacos . [73] Producen daño tisular al causar compresión del tejido por un hematoma o hematomas en expansión. Además, la presión puede provocar una pérdida de suministro de sangre al tejido afectado con el infarto resultante , y la sangre liberada por la hemorragia cerebral parece tener efectos tóxicos directos sobre el tejido cerebral y la vasculatura . [52] [74] La inflamación contribuye a la lesión cerebral secundaria después de la hemorragia. [74]


Stroke is diagnosed through several techniques: a neurological examination (such as the NIHSS), CT scans (most often without contrast enhancements) or MRI scans, Doppler ultrasound, and arteriography. The diagnosis of stroke itself is clinical, with assistance from the imaging techniques. Imaging techniques also assist in determining the subtypes and cause of stroke. There is yet no commonly used blood test for the stroke diagnosis itself, though blood tests may be of help in finding out the likely cause of stroke.[75] In deceased people, an autopsy of stroke may help establishing the time between stroke onset and death.
A physical examination, including taking a medical history of the symptoms and a neurological status, helps giving an evaluation of the location and severity of stroke. It can give a standard score on e.g., the NIH stroke scale.
For diagnosing ischemic (blockage) stroke in the emergency setting:[76]
For diagnosing hemorrhagic stroke in the emergency setting:
For detecting chronic hemorrhages, an MRI scan is more sensitive.[77]
For the assessment of stable stroke, nuclear medicine scans such as single-photon emission computed tomography (SPECT) and positron emission tomography–computed tomography (PET/CT) may be helpful. SPECT documents cerebral blood flow, whereas PET with an FDG isotope shows cerebral glucose metabolism.
CT scans may not detect ischemic stroke, especially if it is small, of recent onset,[10] or in the brainstem or cerebellum areas (posterior circulation infarct). MRI is better at detecting a posterior circulation infarct with diffusion-weighted imaging.[78] A CT scan is used more to rule out certain stroke mimics and detect bleeding.[10] The presence of leptomeningeal collateral circulation in the brain is associated with better clinical outcomes after recanalization treatment.[79] Cerebrovascular reserve capacity is another factor that affects stroke outcome – it is the amount of increase in cerebral blood flow after a purposeful stimulation of blood flow by the physician, such as by giving inhaled carbon dioxide or intravenous acetazolamide. The increase in blood flow can be measured by PET scan or transcranial doppler sonography.[80] However, in people with obstruction of the internal carotid artery of one side, the presence of leptomeningeal collateral circulation is associated with reduced cerebral reserve capacity.[81]
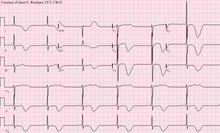
When stroke has been diagnosed, other studies may be performed to determine the underlying cause. With the treatment and diagnosis options available, it is of particular importance to determine whether there is a peripheral source of emboli. Test selection may vary since the cause of stroke varies with age, comorbidity and the clinical presentation. The following are commonly used techniques:
For hemorrhagic stroke, a CT or MRI scan with intravascular contrast may be able to identify abnormalities in the brain arteries (such as aneurysms) or other sources of bleeding, and structural MRI if this shows no cause. If this too does not identify an underlying reason for the bleeding, invasive cerebral angiography could be performed but this requires access to the bloodstream with an intravascular catheter and can cause further stroke as well as complications at the insertion site and this investigation is therefore reserved for specific situations.[82] If there are symptoms suggesting that the hemorrhage might have occurred as a result of venous thrombosis, CT or MRI venography can be used to examine the cerebral veins.[82]
Among people with ischemic stroke, misdiagnosis occurs 2 to 26% of the time.[83] A "stroke chameleon" (SC) is stroke which is diagnosed as something else.[83][84]
People not having stroke may also be misdiagnosed with the condition. Giving thrombolytics (clot-busting) in such cases causes intracerebral bleeding 1 to 2% of the time, which is less than that of people with stroke. This unnecessary treatment adds to health care costs. Even so, the AHA/ASA guidelines state that starting intravenous tPA in possible mimics is preferred to delaying treatment for additional testing.[83]
Women, African-Americans, Hispanic-Americans, Asian and Pacific Islanders are more often misdiagnosed for a condition other than stroke when in fact having stroke. In addition, adults under 44 years of age are seven times more likely to have stroke missed than are adults over 75 years of age. This is especially the case for younger people with posterior circulation infarcts.[83] Some medical centers have used hyperacute MRI in experimental studies for people initially thought to have a low likelihood of stroke, and in some of these people, stroke has been found which were then treated with thrombolytic medication.[83]
Given the disease burden of stroke, prevention is an important public health concern.[85] Primary prevention is less effective than secondary prevention (as judged by the number needed to treat to prevent one stroke per year).[85] Recent guidelines detail the evidence for primary prevention in stroke.[86] About the use of aspirin as a preventive medication for stroke, in healthy people aspirin does not appear beneficial and thus is not recommended,[87] but in people with high cardiovascular risk, or those who have had a myocardial infarction, it provides some protection against a first stroke.[88][89] In those who have previously had stroke, treatment with medications such as aspirin, clopidogrel, and dipyridamole may be beneficial.[88] The U.S. Preventive Services Task Force (USPSTF) recommends against screening for carotid artery stenosis in those without symptoms.[90]
The most important modifiable risk factors for stroke are high blood pressure and atrial fibrillation, although the size of the effect is small; 833 people have to be treated for 1 year to prevent one stroke.[91][92] Other modifiable risk factors include high blood cholesterol levels, diabetes mellitus, end-stage kidney disease,[8] cigarette smoking[93][94] (active and passive), heavy alcohol use,[95] drug use,[96] lack of physical activity, obesity, processed red meat consumption,[97] and unhealthy diet.[98] Smoking just one cigarette per day increases the risk more than 30%.[99] Alcohol use could predispose to ischemic stroke, as well as intracerebral and subarachnoid hemorrhage via multiple mechanisms (for example, via hypertension, atrial fibrillation, rebound thrombocytosis and platelet aggregation and clotting disturbances).[100] Drugs, most commonly amphetamines and cocaine, can induce stroke through damage to the blood vessels in the brain and acute hypertension.[73][101] Migraine with aura doubles a person's risk for ischemic stroke.[102][103] Untreated, celiac disease regardless of the presence of symptoms can be an underlying cause of stroke, both in children and adults.[104] According to a 2021 WHO study, working 55+ hours a week raises the risk of stroke by 35% and the risk of dying from heart conditions by 17%, when compared to a 35-40-hour week.[105]
High levels of physical activity reduce the risk of stroke by about 26%.[106] There is a lack of high quality studies looking at promotional efforts to improve lifestyle factors.[107] Nonetheless, given the large body of circumstantial evidence, best medical management for stroke includes advice on diet, exercise, smoking and alcohol use.[108] Medication is the most common method of stroke prevention; carotid endarterectomy can be a useful surgical method of preventing stroke.
High blood pressure accounts for 35–50% of stroke risk.[109] Blood pressure reduction of 10 mmHg systolic or 5 mmHg diastolic reduces the risk of stroke by ~40%.[110] Lowering blood pressure has been conclusively shown to prevent both ischemic and hemorrhagic stroke.[111][112] It is equally important in secondary prevention.[113] Even people older than 80 years and those with isolated systolic hypertension benefit from antihypertensive therapy.[114][115][116] The available evidence does not show large differences in stroke prevention between antihypertensive drugs—therefore, other factors such as protection against other forms of cardiovascular disease and cost should be considered.[117][118] The routine use of beta-blockers following stroke or TIA has not been shown to result in benefits.[119]
High cholesterol levels have been inconsistently associated with (ischemic) stroke.[112][120] Statins have been shown to reduce the risk of stroke by about 15%.[121] Since earlier meta-analyses of other lipid-lowering drugs did not show a decreased risk,[122] statins might exert their effect through mechanisms other than their lipid-lowering effects.[121]
Diabetes mellitus increases the risk of stroke by 2 to 3 times.[clarification needed][citation needed] While intensive blood sugar control has been shown to reduce small blood vessel complications such as kidney damage and damage to the retina of the eye it has not been shown to reduce large blood vessel complications such as stroke.[123][124]
Oral anticoagulants such as warfarin have been the mainstay of stroke prevention for over 50 years. However, several studies have shown that aspirin and other antiplatelets are highly effective in secondary prevention after stroke or transient ischemic attack.[88] Low doses of aspirin (for example 75–150 mg) are as effective as high doses but have fewer side effects; the lowest effective dose remains unknown.[125] Thienopyridines (clopidogrel, ticlopidine) might be slightly more effective than aspirin and have a decreased risk of gastrointestinal bleeding but are more expensive.[126] Both aspirin and clopidogrel may be useful in the first few weeks after a minor stroke or high-risk TIA.[127] Clopidogrel has less side effects than ticlopidine.[126] Dipyridamole can be added to aspirin therapy to provide a small additional benefit, even though headache is a common side effect.[128] Low-dose aspirin is also effective for stroke prevention after having a myocardial infarction.[89]
Those with atrial fibrillation have a 5% a year risk of stroke, and those with valvular atrial fibrillation have an even higher risk.[129] Depending on the stroke risk, anticoagulation with medications such as warfarin or aspirin is useful for prevention with various levels of comparative effectiveness depending on the type of treatment used.[130][131]
Oral anticoagulants, especially Xa (apixaban) and thrombin (dabigatran) inhibitors, have been shown to be superior to warfarin in stroke reduction and have a lower or similar bleeding risk in patients with atrial fibrillation.[131] Except in people with atrial fibrillation, oral anticoagulants are not advised for stroke prevention—any benefit is offset by bleeding risk.[132]
In primary prevention, however, antiplatelet drugs did not reduce the risk of ischemic stroke but increased the risk of major bleeding.[133][134] Further studies are needed to investigate a possible protective effect of aspirin against ischemic stroke in women.[135][136]
Carotid endarterectomy or carotid angioplasty can be used to remove atherosclerotic narrowing of the carotid artery. There is evidence supporting this procedure in selected cases.[108] Endarterectomy for a significant stenosis has been shown to be useful in preventing further stroke in those who have already had the condition.[137] Carotid artery stenting has not been shown to be equally useful.[138][139] People are selected for surgery based on age, gender, degree of stenosis, time since symptoms and the person's preferences.[108] Surgery is most efficient when not delayed too long—the risk of recurrent stroke in a person who has a 50% or greater stenosis is up to 20% after 5 years, but endarterectomy reduces this risk to around 5%. The number of procedures needed to cure one person was 5 for early surgery (within two weeks after the initial stroke), but 125 if delayed longer than 12 weeks.[140][141]
Screening for carotid artery narrowing has not been shown to be a useful test in the general population.[142] Studies of surgical intervention for carotid artery stenosis without symptoms have shown only a small decrease in the risk of stroke.[143][144] To be beneficial, the complication rate of the surgery should be kept below 4%. Even then, for 100 surgeries, 5 people will benefit by avoiding stroke, 3 will develop stroke despite surgery, 3 will develop stroke or die due to the surgery itself, and 89 will remain stroke-free but would also have done so without intervention.[108]
Nutrition, specifically the Mediterranean-style diet, has the potential to decrease the risk of having a stroke by more than half.[145] It does not appear that lowering levels of homocysteine with folic acid affects the risk of stroke.[146][147]
A number of specific recommendations have been made for women including taking aspirin after the 11th week of pregnancy if there is a history of previous chronic high blood pressure and taking blood pressure medications during pregnancy if the blood pressure is greater than 150 mmHg systolic or greater than 100 mmHg diastolic. In those who have previously had preeclampsia, other risk factors should be treated more aggressively.[148]
Keeping blood pressure below 140/90 mmHg is recommended.[149] Anticoagulation can prevent recurrent ischemic stroke. Among people with nonvalvular atrial fibrillation, anticoagulation can reduce stroke by 60% while antiplatelet agents can reduce stroke by 20%.[150] However, a recent meta-analysis suggests harm from anticoagulation started early after an embolic stroke.[151][152] Stroke prevention treatment for atrial fibrillation is determined according to the CHA2DS2–VASc score. The most widely used anticoagulant to prevent thromboembolic stroke in people with nonvalvular atrial fibrillation is the oral agent warfarin while a number of newer agents including dabigatran are alternatives which do not require prothrombin time monitoring.[149]
Anticoagulants, when used following stroke, should not be stopped for dental procedures.[153]
If studies show carotid artery stenosis, and the person has a degree of residual function on the affected side, carotid endarterectomy (surgical removal of the stenosis) may decrease the risk of recurrence if performed rapidly after stroke.
Stroke, whether ischemic or hemorrhagic, is an emergency that warrants immediate medical attention.[5][154] The specific treatment will depend on the type of stroke, the time elapsed since the onset of symptoms, and the underlying cause or presence of comorbidities.[154]
Aspirin reduces the overall risk of recurrence by 13% with greater benefit early on.[155] Definitive therapy within the first few hours is aimed at removing the blockage by breaking the clot down (thrombolysis), or by removing it mechanically (thrombectomy). The philosophical premise underlying the importance of rapid stroke intervention was summed up as Time is Brain! in the early 1990s.[156] Years later, that same idea, that rapid cerebral blood flow restoration results in fewer brain cells dying, has been proved and quantified.[157]
Tight blood sugar control in the first few hours does not improve outcomes and may cause harm.[158] High blood pressure is also not typically lowered as this has not been found to be helpful.[159][160] Cerebrolysin, a mixture of pig brain-derived neurotrophic factors used widely to treat acute ischemic stroke in China, Eastern Europe, Russia, post-Soviet countries, and other Asian countries, does not improve outcomes or prevent death and may increase the risk of severe adverse events.[161] There is also no evidence that cerebrolysin‐like peptide mixtures which are extracted from cattle brain is helpful in treating acute ischemic stroke.[161]
Thrombolysis, such as with recombinant tissue plasminogen activator (rtPA), in acute ischemic stroke, when given within three hours of symptom onset, results in an overall benefit of 10% with respect to living without disability.[162][163] It does not, however, improve chances of survival.[162] Benefit is greater the earlier it is used.[162] Between three and four and a half hours the effects are less clear.[164][165][166] The AHA/ASA recommend it for certain people in this time frame.[167] A 2014 review found a 5% increase in the number of people living without disability at three to six months; however, there was a 2% increased risk of death in the short term.[163] After four and a half hours thrombolysis worsens outcomes.[164] These benefits or lack of benefits occurred regardless of the age of the person treated.[168] There is no reliable way to determine who will have an intracranial bleed post-treatment versus who will not.[169] In those with findings of savable tissue on medical imaging between 4.5 hours and 9 hours or who wake up with stroke, alteplase results in some benefit.[170]
Its use is endorsed by the American Heart Association, the American College of Emergency Physicians and the American Academy of Neurology as the recommended treatment for acute stroke within three hours of onset of symptoms as long as there are no other contraindications (such as abnormal lab values, high blood pressure, or recent surgery). This position for tPA is based upon the findings of two studies by one group of investigators[171] which showed that tPA improves the chances for a good neurological outcome. When administered within the first three hours thrombolysis improves functional outcome without affecting mortality.[172] 6.4% of people with large stroke developed substantial brain bleeding as a complication from being given tPA thus part of the reason for increased short term mortality.[173] The American Academy of Emergency Medicine had previously stated that objective evidence regarding the applicability of tPA for acute ischemic stroke was insufficient.[174] In 2013 the American College of Emergency Medicine refuted this position,[175] acknowledging the body of evidence for the use of tPA in ischemic stroke;[176] but debate continues.[177][178] Intra-arterial fibrinolysis, where a catheter is passed up an artery into the brain and the medication is injected at the site of thrombosis, has been found to improve outcomes in people with acute ischemic stroke.[179]
Mechanical removal of the blood clot causing the ischemic stroke, called mechanical thrombectomy, is a potential treatment for occlusion of a large artery, such as the middle cerebral artery. In 2015, one review demonstrated the safety and efficacy of this procedure if performed within 12 hours of the onset of symptoms.[180][181] It did not change the risk of death but did reduce disability compared to the use of intravenous thrombolysis, which is generally used in people evaluated for mechanical thrombectomy.[182][183] Certain cases may benefit from thrombectomy up to 24 hours after the onset of symptoms.[184]
Stroke affecting large portions of the brain can cause significant brain swelling with secondary brain injury in surrounding tissue. This phenomenon is mainly encountered in stroke affecting brain tissue dependent upon the middle cerebral artery for blood supply and is also called "malignant cerebral infarction" because it carries a dismal prognosis. Relief of the pressure may be attempted with medication, but some require hemicraniectomy, the temporary surgical removal of the skull on one side of the head. This decreases the risk of death, although some people – who would otherwise have died – survive with disability.[185][186]
People with intracerebral hemorrhage require supportive care, including blood pressure control if required. People are monitored for changes in the level of consciousness, and their blood sugar and oxygenation are kept at optimum levels. Anticoagulants and antithrombotics can make bleeding worse and are generally discontinued (and reversed if possible).[citation needed] A proportion may benefit from neurosurgical intervention to remove the blood and treat the underlying cause, but this depends on the location and the size of the hemorrhage as well as patient-related factors, and ongoing research is being conducted into the question as to which people with intracerebral hemorrhage may benefit.[187]
In subarachnoid hemorrhage, early treatment for underlying cerebral aneurysms may reduce the risk of further hemorrhages. Depending on the site of the aneurysm this may be by surgery that involves opening the skull or endovascularly (through the blood vessels).[188]
Ideally, people who have had stroke are admitted to a "stroke unit", a ward or dedicated area in a hospital staffed by nurses and therapists with experience in stroke treatment. It has been shown that people admitted to stroke units have a higher chance of surviving than those admitted elsewhere in hospital, even if they are being cared for by doctors without experience in stroke.[2][189] Nursing care is fundamental in maintaining skin care, feeding, hydration, positioning, and monitoring vital signs such as temperature, pulse, and blood pressure.[190]
Stroke rehabilitation is the process by which those with disabling stroke undergo treatment to help them return to normal life as much as possible by regaining and relearning the skills of everyday living. It also aims to help the survivor understand and adapt to difficulties, prevent secondary complications, and educate family members to play a supporting role. Stroke rehabilitation should begin almost immediately with a multidisciplinary approach. The rehabilitation team may involve physicians trained in rehabilitation medicine, neurologists, clinical pharmacists, nursing staff, physiotherapists, occupational therapists, speech-language pathologists, and orthotists. Some teams may also include psychologists and social workers, since at least one-third of affected people manifests post stroke depression. Validated instruments such as the Barthel scale may be used to assess the likelihood of a person who has had stroke being able to manage at home with or without support subsequent to discharge from a hospital.[191]
Stroke rehabilitation should be started as quickly as possible and can last anywhere from a few days to over a year. Most return of function is seen in the first few months, and then improvement falls off with the "window" considered officially by U.S. state rehabilitation units and others to be closed after six months, with little chance of further improvement.[medical citation needed] However, some people have reported that they continue to improve for years, regaining and strengthening abilities like writing, walking, running, and talking.[medical citation needed] Daily rehabilitation exercises should continue to be part of the daily routine for people who have had stroke. Complete recovery is unusual but not impossible and most people will improve to some extent: proper diet and exercise are known to help the brain to recover.
The body of evidence is uncertain on the efficacy of cognitive rehabilitation for reducing the disabling effects of neglect and increasing independence remains unproven.[192] However, there is limited evidence that cognitive rehabilitation may have an immediate beneficial effect on tests of neglect.[192] Overall, no rehabilitation approach can be supported by evidence for spatial neglect.
The body of evidence is uncertain whether the use of rehabilitation can improve on-road driving skills following stroke.[193] There is limited evidence that training on a driving simulator will improve performance on recognizing road signs after training.[193] The findings are based on low-quality evidence as further research is needed involving large numbers of participants.
Based on low quality evidence, it is uncertain whether yoga has a significant benefit for stroke rehabilitation on measures of quality of life, balance, strength, endurance, pain, and disability scores.[194] Yoga may reduce anxiety and could be included as part of patient-centred stroke rehabilitation.[194] Further research is needed assessing the benefits and safety of yoga in stroke rehabilitation.
Low-quality evidence suggests that action observation (a type of physiotherapy that is meant to improve neural plasticity through the mirror-neuronal system) may be of some benefit and has no significant adverse effects, however this benefit may not be clinically significant and further research is suggested.[195]
The body of scientific evidence is uncertain on the effectiveness of cognitive rehabilitation for attention deficits in patients following stroke.[196] While there may be an immediate effect after treatment on attention, the findings are based on low to moderate quality and small number of studies.[196] Further research is needed to assess whether the effect can be sustained in day-to-day tasks requiring attention.
The latest evidence supports the short-term benefits of motor imagery (MI) on walking speed in individuals who have had stroke, in comparison to other therapies.[197] MI does not improve motor function after stroke and does not seem to cause significant adverse events.[197] The findings are based on low-quality evidence as further research is needed to estimate the effect of MI on walking endurance and the dependence on personal assistance.
Physical and occupational therapy have overlapping areas of expertise; however, physical therapy focuses on joint range of motion and strength by performing exercises and relearning functional tasks such as bed mobility, transferring, walking and other gross motor functions. Physiotherapists can also work with people who have had stroke to improve awareness and use of the hemiplegic side. Rehabilitation involves working on the ability to produce strong movements or the ability to perform tasks using normal patterns. Emphasis is often concentrated on functional tasks and people's goals. One example physiotherapists employ to promote motor learning involves constraint-induced movement therapy. Through continuous practice the person relearns to use and adapt the hemiplegic limb during functional activities to create lasting permanent changes.[198] Physical therapy is effective for recovery of function and mobility after stroke.[199] Occupational therapy is involved in training to help relearn everyday activities known as the activities of daily living (ADLs) such as eating, drinking, dressing, bathing, cooking, reading and writing, and toileting. Approaches to helping people with urinary incontinence include physical therapy, cognitive therapy, and specialized interventions with experienced medical professionals, however, it is not clear how effective these approaches are at improving urinary incontinence following stroke.[200]
Treatment of spasticity related to stroke often involves early mobilizations, commonly performed by a physiotherapist, combined with elongation of spastic muscles and sustained stretching through different positions.[44] Gaining initial improvement in range of motion is often achieved through rhythmic rotational patterns associated with the affected limb.[44] After full range has been achieved by the therapist, the limb should be positioned in the lengthened positions to prevent against further contractures, skin breakdown, and disuse of the limb with the use of splints or other tools to stabilize the joint.[44] Cold ice wraps or ice packs may briefly relieve spasticity by temporarily reducing neural firing rates.[44] Electrical stimulation to the antagonist muscles or vibrations has also been used with some success.[44] Physical therapy is sometimes suggested for people who experience sexual dysfunction following stroke.[201]
With the prevalence of vision problems increasing with age in stroke patients, the overall effect of interventions for age-related visual problems is uncertain. It is also not sure whether people with stroke respond differently from the general population when treating eye problems.[202] Further research in this area is needed as the body of evidence is very low quality.
Speech and language therapy is appropriate for people with the speech production disorders: dysarthria[203] and apraxia of speech,[204] aphasia,[205] cognitive-communication impairments, and problems with swallowing.
Speech and language therapy for aphasia following stroke improves functional communication, reading, writing and expressive language. Speech and language therapy that is higher intensity, higher dose or provided over a long duration of time leads to significantly better functional communication but people might be more likely to drop out of high intensity treatment (up to 15 hours per week).[206] A total of 20-50 hours of speech and language therapy is necessary for the best recovery. The most improvement happens when 2-5 hours of therapy is provided each week over 4-5 days. Recovery is further improved when besides the therapy people practice tasks at home.[207][208] Speech and language therapy is also effective if it is delivered online through video or by a family member who has been trained by a professional therapist.[207][208]
Recovery with therapy for aphasia is also dependent on the recency of stroke and the age of the person. Receiving therapy within a month after the stroke leads to the greatest improvements. 3 or 6 months after the stroke more therapy will be needed but symptoms can still be improved. People with aphasia who are younger than 55 years are the most likely to improve but people older than 75 years can still get better with therapy.[209][210]
People who have had stroke may have particular problems, such as dysphagia, which can cause swallowed material to pass into the lungs and cause aspiration pneumonia. The condition may improve with time, but in the interim, a nasogastric tube may be inserted, enabling liquid food to be given directly into the stomach. If swallowing is still deemed unsafe, then a percutaneous endoscopic gastrostomy (PEG) tube is passed and this can remain indefinitely. Swallowing therapy has mixed results as of 2018.[211]
Often, assistive technology such as wheelchairs, walkers and canes may be beneficial. Many mobility problems can be improved by the use of ankle foot orthoses.[212]
Stroke can also reduce people's general fitness.[213] Reduced fitness can reduce capacity for rehabilitation as well as general health.[214] Physical exercises as part of a rehabilitation program following stroke appear safe.[213] Cardiorespiratory fitness training that involves walking in rehabilitation can improve speed, tolerance and independence during walking, and may improve balance.[213] There are inadequate long-term data about the effects of exercise and training on death, dependence and disability after stroke.[213] The future areas of research may concentrate on the optimal exercise prescription and long-term health benefits of exercise. The effect of physical training on cognition also may be studied further.
The ability to walk independently in their community, indoors or outdoors, is important following stroke. Although no negative effects have been reported, it is unclear if outcomes can improve with these walking programs when compared to usual treatment.[215]
Some current and future therapy methods include the use of virtual reality and video games for rehabilitation. These forms of rehabilitation offer potential for motivating people to perform specific therapy tasks that many other forms do not.[216] While virtual reality and interactive video gaming are not more effective than conventional therapy for improving upper limb function, when used in conjunction with usual care these approaches may improve upper limb function and ADL function.[217] There are inadequate data on the effect of virtual reality and interactive video gaming on gait speed, balance, participation and quality of life.[217] Many clinics and hospitals are adopting the use of these off-the-shelf devices for exercise, social interaction, and rehabilitation because they are affordable, accessible and can be used within the clinic and home.[216]
Mirror therapy is associated with improved motor function of the upper extremity in people who have had stroke.[218]
Other non-invasive rehabilitation methods used to augment physical therapy of motor function in people recovering from stroke include transcranial magnetic stimulation and transcranial direct-current stimulation.[219] and robotic therapies.[220] Constraint‐induced movement therapy (CIMT), mental practice, mirror therapy, interventions for sensory impairment, virtual reality and a relatively high dose of repetitive task practice may be effective in improving upper limb function. However, further primary research, specifically of CIMT, mental practice, mirror therapy and virtual reality is needed.[221]
Clinical studies confirm the importance of orthoses in stroke rehabilitation.[222][223][224] The orthosis supports the therapeutic applications and also helps to mobilize the patient at an early stage. With the help of an orthosis, physiological standing and walking can be learned again, and late health consequences caused by a wrong gait pattern can be prevented. A treatment with an orthosis can therefore be used to support the therapy.
Stroke can affect the ability to live independently and with quality. Self-management programs are a special training that educates stroke survivors about stroke and its consequences, helps them acquire skills to cope with their challenges, and helps them set and meet their own goals during their recovery process. These programs are tailored to the target audience, and led by someone trained and expert in stroke and its consequences (most commonly professionals, but also stroke survivors and peers). A 2016 review reported that these programs improve the quality of life after stroke, without negative effects. People with stroke felt more empowered, happy and satisfied with life after participating in this training.[225]
Disability affects 75% of stroke survivors enough to decrease their ability to work.[226]Stroke can affect people physically, mentally, emotionally, or a combination of the three. The results of stroke vary widely depending on size and location of the lesion.[227]
Some of the physical disabilities that can result from stroke include muscle weakness, numbness, pressure sores, pneumonia, incontinence, apraxia (inability to perform learned movements), difficulties carrying out daily activities, appetite loss, speech loss, vision loss and pain. If the stroke is severe enough, or in a certain location such as parts of the brainstem, coma or death can result. Up to 10% of people following stroke develop seizures, most commonly in the week subsequent to the event; the severity of the stroke increases the likelihood of a seizure.[228][229] An estimated 15% of people experience urinary incontinence for more than a year following stroke.[200] 50% of people have a decline in sexual function (sexual dysfunction) following stroke.[201]
Emotional and mental dysfunctions correspond to areas in the brain that have been damaged. Emotional problems following stroke can be due to direct damage to emotional centers in the brain or from frustration and difficulty adapting to new limitations. Post-stroke emotional difficulties include anxiety, panic attacks, flat affect (failure to express emotions), mania, apathy and psychosis. Other difficulties may include a decreased ability to communicate emotions through facial expression, body language and voice.[230]
Disruption in self-identity, relationships with others, and emotional well-being can lead to social consequences after stroke due to the lack of ability to communicate. Many people who experience communication impairments after stroke find it more difficult to cope with the social issues rather than physical impairments. Broader aspects of care must address the emotional impact speech impairment has on those who experience difficulties with speech after stroke.[203] Those who experience a stroke are at risk of paralysis, which could result in a self-disturbed body image, which may also lead to other social issues.[231]
30 to 50% of stroke survivors develop post-stroke depression, which is characterized by lethargy, irritability, sleep disturbances, lowered self-esteem and withdrawal.[232] Depression can reduce motivation and worsen outcome, but can be treated with social and family support, psychotherapy and, in severe cases, antidepressants. Psychotherapy sessions may have a small effect on improving mood and preventing depression after stroke.[233] Antidepressant medications may be useful for treating depression after stroke but are associated with central nervous system and gastrointestinal adverse events.[233]
Emotional lability, another consequence of stroke, causes the person to switch quickly between emotional highs and lows and to express emotions inappropriately, for instance with an excess of laughing or crying with little or no provocation. While these expressions of emotion usually correspond to the person's actual emotions, a more severe form of emotional lability causes the affected person to laugh and cry pathologically, without regard to context or emotion.[226] Some people show the opposite of what they feel, for example crying when they are happy.[234] Emotional lability occurs in about 20% of those who have had stroke. Those with a right hemisphere stroke are more likely to have empathy problems which can make communication harder.[235]
Cognitive deficits resulting from stroke include perceptual disorders, aphasia,[236] dementia,[237][238] and problems with attention[239] and memory.[240] Stroke survivors may be unaware of their own disabilities, a condition called anosognosia. In a condition called hemispatial neglect, the affected person is unable to attend to anything on the side of space opposite to the damaged hemisphere. Cognitive and psychological outcome after stroke can be affected by the age at which the stroke happened, pre-stroke baseline intellectual functioning, psychiatric history and whether there is pre-existing brain pathology.[241]
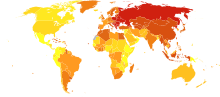

Stroke was the second most frequent cause of death worldwide in 2011, accounting for 6.2 million deaths (~11% of the total).[243] Approximately 17 million people had stroke in 2010 and 33 million people have previously had stroke and were still alive.[19] Between 1990 and 2010 the incidence of stroke decreased by approximately 10% in the developed world and increased by 10% in the developing world.[19] Overall, two-thirds of stroke occurred in those over 65 years old.[19] South Asians are at particularly high risk of stroke, accounting for 40% of global stroke deaths.[244] Incidence of ischemic stroke is ten times more frequent than haemorrhagic stroke.[245]
It is ranked after heart disease and before cancer.[2] In the United States stroke is a leading cause of disability, and recently declined from the third leading to the fourth leading cause of death.[246] Geographic disparities in stroke incidence have been observed, including the existence of a "stroke belt" in the southeastern United States, but causes of these disparities have not been explained.
The risk of stroke increases exponentially from 30 years of age, and the cause varies by age.[247] Advanced age is one of the most significant stroke risk factors. 95% of stroke occurs in people age 45 and older, and two-thirds of stroke occurs in those over the age of 65.[52][232]
A person's risk of dying if he or she does have stroke also increases with age. However, stroke can occur at any age, including in childhood.[citation needed]
Family members may have a genetic tendency for stroke or share a lifestyle that contributes to stroke. Higher levels of Von Willebrand factor are more common amongst people who have had ischemic stroke for the first time.[248] The results of this study found that the only significant genetic factor was the person's blood type. Having stroke in the past greatly increases one's risk of future stroke.
Men are 25% more likely to develop stroke than women,[52] yet 60% of deaths from stroke occur in women.[234] Since women live longer, they are older on average when they have stroke and thus more often killed.[52] Some risk factors for stroke apply only to women. Primary among these are pregnancy, childbirth, menopause, and the treatment thereof (HRT).

Episodes of stroke and familial stroke have been reported from the 2nd millennium BC onward in ancient Mesopotamia and Persia.[249] Hippocrates (460 to 370 BC) was first to describe the phenomenon of sudden paralysis that is often associated with ischemia. Apoplexy, from the Greek word meaning "struck down with violence", first appeared in Hippocratic writings to describe this phenomenon.[250][251]The word stroke was used as a synonym for apoplectic seizure as early as 1599,[252] and is a fairly literal translation of the Greek term. The term apoplectic stroke is an archaic, nonspecific term, for a cerebrovascular accident accompanied by haemorrhage or haemorrhagic stroke.[253] Martin Luther was described as having an apoplectic stroke that deprived him of his speech shortly before his death in 1546.[254]
In 1658, in his Apoplexia, Johann Jacob Wepfer (1620–1695) identified the cause of hemorrhagic stroke when he suggested that people who had died of apoplexy had bleeding in their brains.[52][250]Wepfer also identified the main arteries supplying the brain, the vertebral and carotid arteries, and identified the cause of a type of ischemic stroke known as a cerebral infarction when he suggested that apoplexy might be caused by a blockage to those vessels.[52] Rudolf Virchow first described the mechanism of thromboembolism as a major factor.[255]
The term cerebrovascular accident was introduced in 1927, reflecting a "growing awareness and acceptance of vascular theories and (...) recognition of the consequences of a sudden disruption in the vascular supply of the brain".[256] Its use is now discouraged by a number of neurology textbooks, reasoning that the connotation of fortuitousness carried by the word accident insufficiently highlights the modifiability of the underlying risk factors.[257][258][259] Cerebrovascular insult may be used interchangeably.[260]
The term brain attack was introduced for use to underline the acute nature of stroke according to the American Stroke Association,[260] which has used the term since 1990,[261] and is used colloquially to refer to both ischemic as well as hemorrhagic stroke.[262]
As of 2017, angioplasty and stents were under preliminary clinical research to determine the possible therapeutic advantages of these procedures in comparison to therapy with statins, antithrombotics, or antihypertensive drugs.[263]
{{cite web}}: CS1 maint: bot: original URL status unknown (link){{cite report}}: CS1 maint: DOI inactive as of March 2024 (link)at 3–4.5 hours after stroke onset t-PA increases risk of symptomatic intracranial hemorrhage but effect on functional outcomes is inconsistent[verification needed]