El 31 de diciembre de 2019, China anunció el descubrimiento de un grupo de casos de neumonía en Wuhan . El primer caso estadounidense se informó el 20 de enero [9] y el Secretario de Salud y Servicios Humanos , Alex Azar, declaró una emergencia de salud pública el 31 de enero [10]. Se impusieron restricciones a los vuelos que llegaban desde China [11] [12] pero la respuesta inicial de Estados Unidos a la pandemia fue , por lo demás, lenta en términos de preparar el sistema de atención sanitaria, detener otros viajes y realizar pruebas [13] [14] [15] [a] [17] Las primeras muertes estadounidenses conocidas ocurrieron en febrero [18] y, a fines de febrero, el presidente Donald Trump propuso asignar 2.500 millones de dólares para combatir el brote. En cambio, el Congreso aprobó 8.300 millones de dólares con solo el senador Rand Paul y dos representantes de la Cámara de Representantes ( Andy Biggs y Ken Buck ) votando en contra, y Trump firmó el proyecto de ley, la Ley de Asignaciones Suplementarias de Preparación y Respuesta al Coronavirus de 2020 , el 6 de marzo. [19] Trump declaró una emergencia nacional el 13 de marzo. [20] El gobierno también compró grandes cantidades de equipo médico, invocando la Ley de Producción de Defensa de 1950 para ayudar. [21] A mediados de abril, todos los estados y territorios hicieron declaraciones de desastre, ya que todos tenían casos en aumento. Una segunda ola de infecciones comenzó en junio, luego de que se relajaran las restricciones en varios estados, lo que llevó a que los casos diarios superaran los 60.000. A mediados de octubre, comenzó un tercer aumento de casos; hubo más de 200.000 nuevos casos diarios durante partes de diciembre de 2020 y enero de 2021. [22] [23]
Las vacunas contra la COVID-19 estuvieron disponibles en diciembre de 2020, bajo uso de emergencia, iniciando el programa nacional de vacunación , con la primera vacuna aprobada oficialmente por la Administración de Alimentos y Medicamentos (FDA) el 23 de agosto de 2021. [24] Los estudios han demostrado que son altamente protectoras contra enfermedades graves, hospitalización y muerte. En comparación con las personas completamente vacunadas, los CDC encontraron que aquellos que no estaban vacunados tenían de 5 a casi 30 veces más probabilidades de infectarse u hospitalizarse. No obstante, ha habido cierta vacilación ante las vacunas por varias razones, aunque los efectos secundarios son raros. [25] [26] También hubo numerosos informes de que los pacientes con COVID-19 no vacunados agotaron la capacidad de los hospitales en todo el país , obligando a muchos a rechazar a pacientes con enfermedades potencialmente mortales.
En marzo de 2021 se produjo un cuarto aumento de las infecciones, en medio del auge de la variante Alfa , una variante más fácilmente transmisible detectada por primera vez en el Reino Unido . A esto le siguió un aumento de la variante Delta , una mutación aún más infecciosa detectada por primera vez en la India , lo que llevó a aumentar los esfuerzos para garantizar la seguridad. La aparición en enero de 2022 de la variante Ómicron , que se descubrió por primera vez en Sudáfrica , provocó máximos históricos de hospitalizaciones y casos a principios de 2022, con hasta 1,5 millones de nuevas infecciones notificadas en un solo día. [27] A finales de 2022, se estima que el 77,5% de los estadounidenses habían tenido COVID-19 al menos una vez, según los CDC. [28]
Las respuestas estatales y locales a la pandemia durante la emergencia de salud pública incluyeron el requisito de usar una mascarilla en situaciones específicas (mandatos de mascarilla), la prohibición y cancelación de reuniones a gran escala (incluidos festivales y eventos deportivos), órdenes de quedarse en casa y cierres de escuelas . [29] Se observaron números desproporcionados de casos entre las poblaciones negras y latinas , [30] [31] [32] así como niveles elevados de vacilación ante las vacunas, [33] [34] y hubo un fuerte aumento en los incidentes reportados de xenofobia y racismo contra los estadounidenses de origen asiático . [35] [36] Se produjeron grupos de infecciones y muertes en muchas áreas. [b] La pandemia de COVID-19 también vio el surgimiento de desinformación y teorías conspirativas , [39] y destacó las debilidades en el sistema de salud pública de EE. UU. [17] [40] [41]
En Estados Unidos, ha habido 103.436.829 [3] casos confirmados de COVID-19 con 1.193.165 [3] muertes confirmadas, la mayor cantidad de cualquier país y la 17.ª tasa per cápita más alta del mundo. [42] La pandemia de COVID-19 se clasifica como el desastre más mortal en la historia del país . [43] Fue la tercera causa principal de muerte en los EE. UU. en 2020, detrás de las enfermedades cardíacas y el cáncer. [44] De 2019 a 2020, la esperanza de vida en EE. UU. se redujo en tres años para los hispanos y latinoamericanos , 2,9 años para los afroamericanos y 1,2 años para los estadounidenses blancos . [45] En 2021, las muertes en EE. UU. debido a COVID-19 aumentaron, [46] y la esperanza de vida disminuyó. [47]
En noviembre de 2019, las primeras infecciones por COVID-19 estallaron en Wuhan , China. [48] [49] China informó públicamente del grupo el 31 de diciembre de 2019. [50] Después de que China confirmara que el grupo de infecciones fue causado por un nuevo coronavirus infeccioso [50] el 7 de enero de 2020, los CDC emitieron un aviso sanitario oficial al día siguiente. [51] El 20 de enero, la Organización Mundial de la Salud (OMS) y China confirmaron que se había producido una transmisión de persona a persona. [52] Los CDC activaron inmediatamente su centro de operaciones de emergencia (COE) para responder al brote en China. [53] Además, se informó públicamente del primer informe de un caso de COVID-19 en los EE. UU., [50] aunque el estudio All of Us (publicado en 2021) mostró que cinco estados ya tenían casos semanas antes. [54] Después de que se reportaran otros casos, el 30 de enero, la OMS declaró una emergencia de salud pública de interés internacional (ESPII) - su nivel más alto de alarma [55] - advirtiendo que "todos los países deben estar preparados para la contención". [56] [57] [e] El mismo día, el CDC confirmó el primer caso de persona a persona en los EE. UU. [59] Al día siguiente, el país declaró una emergencia de salud pública. [60] Aunque para esa fecha solo había siete casos conocidos en los EE. UU., el HHS y el CDC informaron que existía la posibilidad de que aparecieran más casos en el país. [60]
En enero, la administración Trump evacuó a ciudadanos estadounidenses de Wuhan. [61] El 2 de febrero, Estados Unidos promulgó restricciones de viaje hacia y desde China. [12] El 6 de febrero, la primera muerte estadounidense confirmada por COVID-19 (la de una mujer de 57 años) ocurrió en el condado de Santa Clara, California . Los CDC no informaron su confirmación hasta el 21 de abril, [62] momento en el que se habían producido otras nueve muertes por COVID-19 en el condado de Santa Clara. [63] El virus había estado circulando sin ser detectado al menos desde principios de enero y posiblemente ya en noviembre. [64]
El 25 de febrero, el CDC advirtió por primera vez al público estadounidense que se preparara para un brote local. [65] [66] Al día siguiente, la ciudad de Nueva York vio enfermarse a su "paciente cero", el abogado de Manhattan Lawrence Garbuz, que entonces se pensaba que era el primer caso adquirido en la comunidad. [67] [68] [69] Otro caso conocido como "paciente cero" en Los Ángeles es un hombre llamado Gregg Garfield, que pasó 64 días en el Hospital de Burbank, con un respirador durante 30 días, con un 1% de posibilidades de vivir. Al contraer el virus en un viaje de esquí, Garfield pudo regresar a las pistas, aunque con algunos dedos de las manos y de los pies amputados. [70]
En febrero, el vicepresidente Mike Pence reemplazó al secretario del HHS Alex Azar como presidente del Grupo de Trabajo sobre el Coronavirus de la Casa Blanca , y Trump dijo: "Estamos muy, muy preparados para esto, para cualquier cosa, ya sea que se trate de un brote de proporciones mayores o de que estemos en ese nivel muy bajo". [71] A fines de febrero, Trump propuso asignar $2.5 mil millones para combatir el brote, pero el Congreso aprobó $8.3 mil millones con solo el senador Rand Paul y los representantes Andy Biggs y Ken Buck votando en contra, y Trump firmó el proyecto de ley el 6 de marzo. [19]
.jpg/440px-President_Trump_Signs_the_Congressional_Funding_Bill_for_Coronavirus_Response_(49627907646).jpg)
Para el 11 de marzo, el virus se había propagado a 110 países y la OMS declaró oficialmente una pandemia . [29] Los CDC ya habían advertido que un gran número de personas que necesitaran atención hospitalaria podrían sobrecargar el sistema de salud, lo que provocaría muertes que de otro modo se podrían prevenir. [72] [73] El director del Instituto Nacional de Alergias y Enfermedades Infecciosas, Anthony Fauci , dijo que la mortalidad por COVID-19 era diez veces mayor que la de la gripe común . [74] Para el 12 de marzo, los casos diagnosticados de COVID-19 en los EE. UU. superaron los mil. [75] Trump declaró una emergencia nacional el 13 de marzo. [20] El 16 de marzo, la Casa Blanca desaconsejó cualquier reunión de más de diez personas. [76] Tres días después, el Departamento de Estado de los Estados Unidos aconsejó a los ciudadanos estadounidenses que evitaran todos los viajes internacionales. [77]
A mediados de marzo, los cincuenta estados podían realizar pruebas con la aprobación de un médico, ya sea de los CDC o de laboratorios comerciales. Sin embargo, la cantidad de kits de prueba disponibles seguía siendo limitada. [78] A medida que los casos comenzaron a propagarse por todo el país, las agencias federales y estatales comenzaron a tomar medidas urgentes para prepararse para un aumento repentino de pacientes hospitalizados. Una de las acciones fue establecer lugares adicionales para pacientes en caso de que los hospitales se vieran desbordados. [79]
A lo largo de marzo y principios de abril, varios gobiernos estatales, municipales y de condado impusieron cuarentenas de "quedarse en casa" a sus poblaciones para detener la propagación del virus. [80] Para el 26 de marzo, los datos del New York Times mostraron que Estados Unidos tenía el mayor número de casos conocidos de cualquier país. [81] Para el 27 de marzo, el país había reportado más de 100.000 casos. [82] El 2 de abril, por orden del presidente Trump, los Centros de Servicios de Medicare y Medicaid (CMS) y los CDC ordenaron pautas preventivas adicionales para la industria de los centros de atención a largo plazo. [83] El 11 de abril, el número de muertos en Estados Unidos se convirtió en el más alto del mundo cuando el número de muertes alcanzó las 20.000, superando al de Italia . [84] El 19 de abril, el CMS agregó nuevas regulaciones que requieren que los hogares de ancianos informen a los residentes, sus familias y representantes, de los casos de COVID-19 en sus instalaciones. [85] El 28 de abril, el número total de casos confirmados en todo el país superó el millón. [86]
Para el 27 de mayo, menos de cuatro meses después de que la pandemia llegara a los EE. UU., 100.000 estadounidenses habían muerto a causa de la COVID-19. [87] La reapertura económica de los estados y la falta de órdenes generalizadas de uso de mascarillas dieron lugar a un marcado aumento de los casos en la mayor parte del territorio continental de los EE. UU., fuera del noreste. [88] Un estudio realizado en mayo de 2020 indicó que el número real de casos de COVID-19 en los Estados Unidos era mucho mayor que el número de casos confirmados, y que en algunos lugares había entre 6 y 24 veces más infecciones, lo que se confirmó aún más mediante una encuesta serológica posterior a nivel de población. [89] [90] [91]
El 6 de julio, el Departamento de Estado de los Estados Unidos anunció la retirada del país de la OMS a partir del 6 de julio de 2021. [92] El 10 de julio, los CDC adoptaron la tasa de letalidad por infección (IFR), "el número de personas que mueren a causa de la enfermedad entre todas las personas infectadas (sintomáticas y asintomáticas)", como una nueva métrica para la gravedad de la enfermedad. [93] En julio, el PIRG de EE. UU. y 150 profesionales de la salud enviaron una carta pidiendo al gobierno federal que "lo cerrara ahora y comenzara de nuevo". [94] En julio y principios de agosto, las solicitudes se multiplicaron, y varios expertos pidieron confinamientos de "seis a ocho semanas" [95] que creían que restablecerían el país el 1 de octubre, a tiempo para reabrir las escuelas y tener una elección en persona. [96]
En agosto, más de 400.000 personas asistieron al 80.º Rally de motocicletas de Sturgis en Sturgis, Dakota del Sur , y desde allí, al menos 300 personas en más de 20 estados se infectaron. [97] Los CDC hicieron un seguimiento con un informe sobre los 51 casos primarios confirmados asociados al evento, 21 casos secundarios y cinco casos terciarios en el estado vecino de Minnesota, donde un asistente murió de COVID-19. [98] Estados Unidos superó los cinco millones de casos de COVID-19 el 8 de agosto. [99]
El 22 de septiembre, Estados Unidos superó las 200.000 muertes, según datos de la Universidad Johns Hopkins. [100] A principios de octubre, una serie sin precedentes de figuras políticas estadounidenses de alto perfil y miembros de su personal anunciaron que habían dado positivo por COVID-19. [101] [102] El 2 de octubre, Trump anunció en Twitter que tanto él como la Primera Dama habían dado positivo por COVID-19 y que se pondrían en cuarentena de inmediato. [103] [102] A Trump le dieron un producto experimental de Regeneron con dos anticuerpos monoclonales [104] [f] y lo llevaron al Centro Médico Militar Nacional Walter Reed , [106] donde le administraron remdesivir y dexametasona . [107]
USA Today estudió las consecuencias de la campaña electoral presidencial y reconoció que era imposible determinar la causalidad. Entre sus hallazgos, los casos aumentaron un 35 por ciento en comparación con el 14 por ciento del estado después de un mitin de Trump en el condado de Beltrami, Minnesota . Un caso se relacionó con unmitin de Joe Biden en Duluth, Minnesota . [108]
El 9 de noviembre, el equipo de transición del presidente electo Biden anunció su Junta Asesora de COVID-19 . [109] El mismo día, el número total de casos había superado los diez millones [110] mientras que el total había aumentado en más de un millón en los diez días anteriores, con un promedio de 102.300 casos nuevos por día. [111] Pfizer también anunció que su vacuna COVID-19 puede tener hasta un noventa por ciento de efectividad. [112] [113] En noviembre, la administración Trump llegó a un acuerdo con varios puntos de venta minorista, incluidas farmacias y supermercados, para que la vacuna COVID-19 fuera gratuita una vez que estuviera disponible. [114]
A pesar de las recomendaciones del gobierno de no viajar, más de 2 millones de personas volaron en aerolíneas durante el período de Acción de Gracias. [115] El 8 de diciembre, Estados Unidos superó los 15 millones de casos, y aproximadamente uno de cada 22 estadounidenses dio positivo desde que comenzó la pandemia. [116] El 14 de diciembre, Estados Unidos superó las 300.000 muertes, lo que representa un promedio de más de 961 muertes por día desde la primera muerte conocida el 6 de febrero. Se informaron más de 50.000 muertes en el último mes, con un promedio de 2.403 muertes diarias ocurridas en la última semana. [117]
El 24 de diciembre, tras las preocupaciones sobre una nueva variante del SARS-CoV-2 probablemente más fácilmente transmisible procedente del Reino Unido , posteriormente llamada Alpha, los CDC anunciaron requisitos de pruebas para los pasajeros estadounidenses que viajen desde el Reino Unido , que se administrarán dentro de las 72 horas, a partir del 28 de diciembre. [118] [119] El 29 de diciembre, EE. UU. informó el primer caso de esta variante en Colorado. El paciente no tenía antecedentes de viajes, lo que llevó a los CDC a decir: "Dada la pequeña fracción de infecciones estadounidenses que se han secuenciado, la variante ya podría estar en los Estados Unidos sin haber sido detectada". [120]
.jpg/440px-President_Joe_Biden_visits_Walter_Reed_(03).jpg)
El 1 de enero de 2021, Estados Unidos superó los 20 millones de casos, lo que representa un aumento de más de un millón en la última semana y de 10 millones en menos de dos meses. [121] [122] El 6 de enero, los CDC anunciaron que habían encontrado al menos 52 casos confirmados de la variante Alpha, y también destacaron que ya podría haber más casos en el país. [123] En los días siguientes, se notificaron más casos de la variante en otros estados, lo que llevó al exdirector de los CDC, Tom Frieden, a expresar su preocupación de que Estados Unidos se enfrentará pronto a "un escenario cercano al peor de los casos". [124] Se creía que la variante había estado presente en Estados Unidos desde octubre. [125]
El 19 de enero, Estados Unidos superó las 400.000 muertes, solo cinco semanas después de que el país superara las 300.000 muertes. [126] El 22 de enero, Estados Unidos superó los 25 millones de casos, y uno de cada 13 estadounidenses dio positivo en la prueba de COVID-19. [127] El 29 de enero, los CDC y la Administración de Seguridad del Transporte federal emitieron un requisito nacional para el uso de mascarillas en el transporte público y otras formas de transporte público , que entrará en vigor el 1 de febrero. [128] [129] (Posteriormente, ampliado, el mandato federal de uso de mascarillas para el transporte público sigue vigente en abril de 2022). [129] [130]
El 22 de febrero, Estados Unidos superó las 500.000 muertes, solo cinco semanas después de que el país superara las 400.000 muertes. [131] Para el 5 de marzo, se detectaron más de 2.750 casos de variantes de COVID-19 en 47 estados; Washington, DC; y Puerto Rico . [132] En el primer discurso en horario de máxima audiencia de su presidencia, el 11 de marzo, Biden anunció su plan de presionar a los estados para que pongan las vacunas a disposición de todos los adultos antes del 1 de mayo, con el objetivo de hacer posibles las pequeñas reuniones antes del 4 de julio . [133] El 24 de marzo, Estados Unidos superó los 30 millones de casos, justo cuando varios estados comenzaron a ampliar la edad de elegibilidad para las vacunas COVID-19. [134] Los expertos comenzaron a advertir contra la relajación pública de las medidas de mitigación de COVID-19 a medida que se siguen administrando vacunas, y la directora de los CDC, Rochelle Walensky , advirtió sobre un nuevo aumento de casos. [135]
Para el 7 de abril, la variante Alpha se había convertido en la cepa dominante de COVID-19 en los EE. UU. [136] El 12 de abril, EE. UU. informó sus primeros casos de una nueva variante "doble mutante" del SARS-CoV-2 de la India , más tarde llamada Delta, en California. [137] Para el 25 de abril, se informó que el promedio de siete días de nuevas infecciones del país estaba disminuyendo, pero se plantearon preocupaciones sobre las caídas en la demanda de vacunas en ciertas partes de los EE. UU., que se atribuyeron a la vacilación ante las vacunas . [138] [139] [140] El 29 de abril, los CDC estimaron que aproximadamente el 35% de la población estadounidense había sido infectada con el virus hasta marzo de 2021, aproximadamente cuatro veces más que las cifras oficiales informadas. [141]
El 4 de mayo, Biden anunció un nuevo objetivo: que el 70 por ciento de todos los adultos en Estados Unidos reciban al menos una dosis de la vacuna contra la COVID-19 antes del 4 de julio, junto con medidas para vacunar a los adolescentes y a las poblaciones más inaccesibles. [142] El país finalmente no alcanzó esa meta, ya que solo el 67 por ciento de la población adulta en general lo había hecho antes del 4 de julio . [143] El 6 de mayo, un estudio del Instituto de Métricas y Evaluación de la Salud estimó que la verdadera cifra de muertos por COVID-19 en Estados Unidos era de más de 900.000 personas. [144] El 9 de mayo, el Dr. Fauci confirmó que probablemente la cifra de muertos en Estados Unidos estaba subestimada. [145]
El 13 de mayo, los CDC cambiaron sus directrices y dijeron que las personas completamente vacunadas no necesitan usar mascarillas en la mayoría de las situaciones. [146] Algunos estados terminaron sus mandatos de uso de mascarillas poco después, mientras que otros mantuvieron el mandato. Los CDC fueron criticados por la confusión resultante del anuncio, ya que no eliminaron los mandatos estatales y locales existentes. Las directrices tampoco eliminaron el mandato federal de uso de mascarillas en el transporte público. [147] El 15 de junio, Estados Unidos superó las 600.000 muertes, aunque el número de muertes diarias había disminuido debido a los esfuerzos de vacunación. [148]
En junio, los casos de COVID-19 volvieron a aumentar, especialmente en Arkansas, Nevada, Missouri y Wyoming. Se cree que el aumento de las cifras se debió a la variante Delta. [149] Para el 7 de julio, la variante Delta había superado a la variante Alpha y se convirtió en la cepa dominante de COVID-19 en los EE. UU., según datos de los CDC. [150] En agosto, la variante Delta representaba el 99 por ciento de todos los casos y se descubrió que duplicaba el riesgo de hospitalización para quienes aún no estaban vacunados. [151]
El 1 de agosto, Estados Unidos superó los 35 millones de casos. [152] A principios y mediados de agosto, los hospitales de algunos estados con bajas tasas de vacunación comenzaron a superar su capacidad. [153] Una cuarta parte de la población estadounidense reside en ocho estados (Alabama, Arkansas, Florida, Georgia, Luisiana, Misisipi, Nevada y Texas), pero, a mediados de agosto, estos estados en conjunto tenían la mitad de las hospitalizaciones por COVID-19 en el país. [154] A fines de mes, las UCI de cinco de ellos (Alabama, Arkansas, Florida, Georgia y Texas) estaban llenas en más del 90 %. [155]
El 8 de septiembre, Estados Unidos superó los 40 millones de casos. [156] Para el 15 de septiembre, uno de cada 500 estadounidenses había muerto por COVID-19. [157] Para el 20 de septiembre, COVID-19 había matado a más de 675.000 estadounidenses, el número estimado de muertes estadounidenses por la gripe española en 1918. Como resultado, COVID-19 se convirtió en la pandemia respiratoria más mortal en la historia estadounidense reciente. [158] Associated Press calificó las nuevas cifras como una "tragedia colosal" porque, a pesar de un siglo de avances en la ciencia, el país no aprovechó al máximo las vacunas. [159] El 1 de octubre, Estados Unidos superó las 700.000 muertes. [160] El 18 de octubre, Estados Unidos superó los 45 millones de casos. [161] El 26 de noviembre, Biden anunció que Estados Unidos restringirá los viajes desde Sudáfrica y otros siete países africanos debido a las preocupaciones por una nueva variante de la zona , llamada Ómicron. [162]
A principios de enero de 2022, el número de casos por día superó el millón. [163] Al 1 de febrero, las tasas de mortalidad eran un 63% más altas en los EE. UU. que en otros grandes países ricos, debido en parte a tasas de vacunación mucho más bajas en comparación con esos países. [164] El 9 de marzo, la administración Biden informó al Congreso sobre la falta de fondos para pruebas, terapias y vacunas, pero los republicanos continuaron bloqueando nuevos gastos para la pandemia, por lo que los demócratas eliminaron un paquete de ayuda de emergencia de un proyecto de ley de gastos. [165] El 20 de marzo, el Dr. Anthony S. Fauci advirtió sobre un "repunte" de casos como el que había visto Europa recientemente, afirmando que Estados Unidos debería "estar preparado para la posibilidad de que podamos tener otra variante". [166]
En abril de 2022, la CNN informó que las cifras de COVID-19 alcanzaron mínimos pandémicos en todo Estados Unidos, lo que provocó que muchos centros de pruebas cerraran sus puertas. Dado que los centros de pruebas registraban cifras de un solo dígito por día, la directora de la División de Servicios de Salud Pública de la Agencia de Salud y Servicios Humanos del Condado de Haywood en Carolina del Norte, Sarah Henderson, sugirió que esperaba que la mayoría de los condados vieran cierres pronto, si no lo habían hecho ya. "Vimos un exceso de 100 pacientes en nuestro centro de pruebas en los primeros días [de enero], lo que no parece mucho, pero nuestra comunidad es muy pequeña", dijo Henderson. "Las últimas dos semanas, hemos visto cifras de un solo dígito todos los días. Ciertamente no hablaré por otros condados, pero creo que probablemente nos encaminamos hacia esa dirección en la que, si no cierran, están reduciendo las horas y el personal". [167]
El 18 de abril de 2022, la jueza federal de distrito Kathryn Kimball Mizelle , designada por Trump para Florida, puso fin a nivel nacional al mandato federal de uso de mascarillas en el transporte, que la administración Biden había extendido hasta el 3 de mayo siguiendo el consejo de los CDC . [168] El Departamento de Justicia impugnó el fallo varios días después, pero las mascarillas siguieron siendo opcionales en aviones, autobuses y sistemas de metro, excepto cuando lo exigieran los mandatos locales. [169]
La primera Semana Nacional Anual de Conmemoración y Acción por la COVID se celebró del 24 al 30 de abril, y los alcaldes y otros funcionarios políticos declararon la semana de conmemoración en sus respectivas jurisdicciones como parte de un movimiento nacional liderado por una colección de grupos de defensa de la COVID. [170] [171] Según los datos recopilados por NBC News, el número de muertos en Estados Unidos alcanzó el millón el 4 de mayo de 2022, la mayor cifra de muertos registrada en un solo país, seguido de Brasil, con alrededor de 660.000 muertes. [172] La Casa Blanca confirmó la marca del millón con una proclamación presidencial el 12 de mayo, ordenando que las banderas ondearan a media asta en todas las instalaciones federales hasta el anochecer del 16 de mayo. [173]
En junio, Estados Unidos concluyó el proceso de aprobación para la vacunación de niños menores de cinco años, y se espera que las primeras vacunas se administren el 21 de junio. [174] El 12 de junio, Estados Unidos eliminó los requisitos de pruebas de COVID para los viajeros aéreos internacionales entrantes, mientras que los requisitos de vacunación se mantuvieron en gran medida vigentes para los viajeros entrantes que utilicen cualquier modo de transporte transfronterizo. [175]
El número de casos durante los meses de enero a junio de 2022 fue aproximadamente 2,4 veces el número del mismo período en 2021, y el número de muertes atribuidas a COVID también promedió 0,74 veces el número en 2021. [163] No obstante, al 14 de julio, solo 21 estados tienen órdenes de emergencia activas por COVID-19, [176] y todavía no hay requisitos de uso de mascarillas a nivel estatal. [177]
El número de casos en julio y agosto de 2022 fue de 3.672.358 y 3.154.320, respectivamente, con 11.963 y 15.943 muertes atribuidas a COVID, respectivamente. Los totales de estos dos meses reflejan aproximadamente 1,6 veces el número de casos y 0,81 veces el número de muertes de los mismos meses de 2021. [163]
El 18 de septiembre de 2022, en una aparición en 60 Minutes , el presidente Joe Biden declaró su creencia de que la pandemia de COVID-19 había "terminado" en los Estados Unidos. [178] [179] Esta evaluación generó cierto debate en la comunidad médica: en ese momento, Estados Unidos tenía aproximadamente 400 muertes por la enfermedad por día, y cuando se extrapola a 150.000 por año es tres veces la tasa de mortalidad de una mala temporada de gripe . [180]
El número de casos durante los meses de julio a septiembre de 2022 fue aproximadamente 0,86 veces el número del mismo período en 2021, y el número de muertes atribuidas a COVID también promedió 0,42 veces el número del mismo período en 2021. [163]
In October, new variants BQ.1 and BQ.1.1 from the dominant BA.5 appeared to be spreading quickly, but comprised only a small proportion of overall variants. Although variant XBB was of concern internationally, it was rare in the United States.[181] Recommendations for receiving vaccination booster shots are mixed: while populations at risk of severe disease and death should stay up-to-date, healthy, middle-aged-and-younger populations are rarely at risk of severe illness, and most have adequate immunity. Although the newest bivalent boosters target the recent BA.4 and BA.5 variants and their risks are low, some experts recommend new strategies to develop vaccines with broader effectiveness.[182]
In a survey of vaccination booster intake (after completing a primary series), about 15% reported receiving the updated booster. The rates varied racially with 19% among White, non-Hispanic people, about 11% among Hispanic people, and about 7% among non-Hispanic American Indians, Alaska Native people, Black people, and those of multiple races, leading to concerns of vaccination access inequity.[183]
In the months leading up to November, deaths from COVID-19 substantially decreased, attributed to high levels of population immunity (through vaccination or prior infection), and improvements in early treatment for patients at risk for severe disease. The CDC recommended vaccinations, treatments for immunocompromised individuals and to reduce severity of the disease, and continuing to wear masks in public.[184] Nonetheless, Dr. Anthony Fauci stated that the Biden administration felt that there was "enough community protection that we're not going to see a repeat of what we saw last year at this time," referring to the emergence of the Omicron variant.[185]
A study of vaccine effectiveness found that U.S.-authorized bivalent mRNA boosters administered to those having already received 2 to 4 monovalent vaccinations provided significant additional protection against symptomatic SARS-CoV-2.[186] Concerns of a surge in Beijing caused the Biden administration to require U.S. visitors from China, Hong Kong, and Macau to provide proof of COVID-19 negative test results.[187] At the end of the year, the CDC reported that the COVID Omicron XBB.1.5 variant became much more prevalent and represented about 41% of new cases in the U.S. Scientists at Columbia University warned that the rise of subvariants could "result in a surge of breakthrough infections as well as re-infections."[188]
On January 11, 2023, the Biden administration decided to renew the COVID-19 public health emergency amid a winter surge of cases related to highly transmissible Omicron subvariants. With relief measures such as automatic Medicaid re-enrollment being decoupled from the emergency declaration, some commentators believed this signaled the final extension of the emergency declaration.[189]
Although some states had already ended emergency SNAP benefits enacted during the pandemic, the USDA announced that emergency allotments for the remaining 32 states, the District of Columbia, Guam, and the U.S. Virgin Islands would end after the February 2023 distribution. Leaders of some anti-hunger organizations believed that the end of the $95-per-month additional benefit would strain local food pantries and food banks.[190] South Carolina, which ended emergency food grants after the January 2023 distribution, and the 17 other states which terminated pandemic food supplements prior to the federal end date were all states with Republican-controlled state legislatures.[191]
On January 31, 2023, President Biden announced the end to the COVID-19 emergency declarations by May 11, 2023.[192] By February 23, eighteen states had already cut payments for more than 10 million people, and Congress had decided to end the program early, exchanging additional benefits for a new permanent program that provides extra money to low-income families to replace school meals during the summer.[193]
On April 10, 2023, President Biden signed into law a resolution terminating the national emergency, effective immediately.[194][195] This national emergency was separate from the public health emergency, which remained in effect until May 11, 2023.[194]
A late-summer wave of COVID-19 cases, as reflected by tests at pharmacies and healthcare settings, marked the first US surge of infections since the end of the public health emergency. Wastewater testing initially indicated that the uptick in cases was only a third the size of the previous summer's surge, yet data from Walgreens showed the first week of August having the largest number of positive cases since May 2021.[196][197]
Hospitals across the United States reported a 24% rise in hospitalizations during the first two weeks of August and wastewater testing showed increased cases in the West and Northeast. With the pandemic legally declared over earlier in 2023, schools and workplaces responded to outbreaks differently, with many schools seeking to be more judicious about when to keep students home from school. The film studio Lionsgate, however, briefly reinstated a mask mandate following an outbreak, as did Morris Brown College, which also reinstated temperature checks and a restriction on large events for two weeks, at the beginning of the fall 2023 semester.[198] As more schools launched their fall semesters in late August and early September, high positivity rates among students and staff led to temporary in-person learning suspensions across three school districts in Texas and Tennessee, driven by district-level decisions rather than state authorities.[199]
With hospitalizations in excess of 20,000 for the first time since the end of the public health emergency, the federal government restarted the national free COVID test delivery program on September 25, 2023, enabling the delivery of four free COVID-19 tests per mailing address at a time when many insurance providers had begun to drop coverage of COVID tests.[200] The program, entering its fifth round of distributions with the fall 2023 initiative, was suspended in May 2023 to preserve supplies yet Health Secretary Xavier Becerra stated that the stockpile had been replenished and that the program would continue through the holiday season, and beyond, if cases continued to rise. Some of the newly mailed tests would show expired dates on their packaging but would remain valid for testing since the FDA had recently extended the expiration dates of a variety of tests.[201]
Upon entering the first winter season of the post-pandemic period, some health facilities in California, New York, Massachusetts, and Illinois began to reinstate mask mandates for staff and visitors, due to increased rates of infection amid what had become an annual winter milieu of COVID, flu, and RSV.[202] New York City Health and Hospitals resumed its mandate shortly after Christmas, with the additional goal of minimizing staffing shortages throughout the healthcare system.[203]
In January 2024, wastewater data showed that U.S. infections had reached their second-highest recorded level, surpassed only by the initial Omicron wave in January 2022.[204]
Due to a 38% rise in COVID-related hospitalizations in December, rapidly rising RSV infections, and similarly trending flu cases, the city of Saint Louis reinstated a mask mandate for city employees which would have started on January 5. Missouri's Republican governor, a staunch opponent of mask mandates, pressured the city to cancel the mandate less than 24 hours after it had been issued, with the city also revising its previous data on RSV and flu infections.[205]
Meanwhile, the New York City Fire Department instituted a more targeted municipal employee mandate on January 12, which required only firetruck and ambulance personnel to be masked, specifically while rendering pre-hospital patient care. This followed a renewed mask mandate which went into effect at all New York City Health + Hospitals on January 1.[206]
On January 9, in a bid to avoid school and workplace disruptions amid the post-pandemic winter surge, California health officials shortened the recommended period of isolation to one day for infected individuals who exhibit only mild symptoms.[207] On March 1, 2024, the CDC followed suit and shortened its recommended isolation period to one day after being fever-free without the aid of medications, which was the same recommendation provided for influenza and respiratory syncytial virus. The CDC still recommended enhanced precautions, such as wearing a mask and limiting close contact with others, for five days.[208]
On January 28, 2020, the CDC updated its China travel recommendations to level 3, its highest alert.[209] On February 8, the WHO's director-general announced that a team of international experts had been assembled to travel to China and he hoped officials from the CDC would also be part of that mission.[210][211] In January, Boeing announced a donation of 250,000 medical masks to help address China's supply shortages.[212] On February 7, the State Department said it had facilitated the transportation of nearly eighteen tons of medical supplies to China, including masks, gowns, gauze, respirators, and other vital materials.[213] On the same day, U.S. Secretary of State Pompeo announced a $100 million pledge to China and other countries to assist with their fights against the virus.[214]
Contact tracing is a tool to control transmission rates during the reopening process. Some states like Texas and Arizona opted to proceed with reopening without adequate contact tracing programs in place. Health experts have expressed concerns about training and hiring enough personnel to reduce transmission. Privacy concerns have prevented measures such as those imposed in South Korea where authorities used cellphone tracking and credit card details to locate and test thousands of nightclub patrons when new cases began emerging.[215] Funding for contact tracing is thought to be insufficient, and even better-funded states have faced challenges getting in touch with contacts. Congress allocated $631 million for state and local health surveillance programs, but the Johns Hopkins Center for Health Security estimates that $3.6 billion will be needed. The cost rises with the number of infections, and contact tracing is easier to implement when the infection count is lower. Health officials are also worried that low-income communities will fall further behind in contact tracing efforts which "may also be hobbled by long-standing distrust among minorities of public health officials".[216] As of July 1, 2020, only four states were using contact tracing apps as part of their state-level strategies to control transmission. The apps document digital encounters between smartphones, so the users will automatically be notified if someone they had contact with has tested positive. Public health officials in California claim that most of the functionality could be duplicated by using text, chat, email, and phone communications.[217]
In the United States, remdesivir is indicated for use in adults and adolescents (aged twelve years and older with body weight at least 40 kilograms (88 lb)) for the treatment of COVID-19 requiring hospitalization.[218] The FDA issued an emergency use authorization (EUA) for the combination of baricitinib with remdesivir, for the treatment of suspected or laboratory confirmed COVID-19 in hospitalized people two years of age or older requiring supplemental oxygen, invasive mechanical ventilation, or extracorporeal membrane oxygenation (ECMO).[219] In early March, President Trump directed the FDA to test certain medications to discover if they had the potential to treat COVID-19 patients.[220] Among those were chloroquine and hydroxychloroquine, which have been successfully used to treat malaria for over fifty years. A small test in France by researcher Didier Raoult had given positive results, although the study was criticized for design flaws, small sample size, and the fact that it was published before peer review.[221] On March 28, the FDA issued an Emergency Use Authorization (EUA) which allowed certain hospitalized COVID-19 patients to be treated with hydroxychloroquine or chloroquine.[222][220][223][224] On June 15, the FDA revoked the EUA for hydroxychloroquine and chloroquine as potential treatments for COVID-19, saying the available evidence showed "no benefit for decreasing the likelihood of death or speeding recovery".[225] However, Trump continued to promote the use of hydroxychloroquine for COVID-19 through July.[226]
From early 2020, more than 70 companies worldwide (with five or six operating primarily in the U.S.) began vaccine research.[227][228] In preparation for large-scale production, Congress set aside more than $3.5 billion for this purpose as part of the CARES Act.[229][228] On November 20, 2020, the Pfizer–BioNTech partnership submitted a request for emergency use authorization for its vaccine to the Food and Drug Administration (FDA),[230][231] which was granted on December 11.[232][233] On December 18, 2020, the FDA granted the Moderna vaccine emergency use authorization,[234][235] which Moderna had requested on November 30, 2020.[236][237] Starting on December 14, 2020, the first doses of COVID-19 vaccine were administered.[238]
Polling showed a significant partisan divide regarding the outbreak.[239] In February 2020, similar numbers of Democrats and Republicans believed COVID-19 was "a real threat": 70% and 72%, respectively. By mid-March 2020, 76% of Democrats viewed COVID-19 as "a real threat", while only 40% of Republicans agreed.[240] In mid-March, various polls found Democrats were more likely than Republicans to believe "the worst was yet to come" (79–40%), to believe their lives would change in a major way due to the outbreak (56–26%),[241] and to take certain precautions against the virus (83–53%).[242] The CDC was the most trusted source of information about the outbreak (85%), followed by the WHO (77%), state and local government officials (70–71%), the news media (47%), and Trump (46%).[242] A May 2020 poll concluded that 54% of people in the U.S. felt the federal government was doing a poor job in stopping the spread of COVID-19 in the country. 57% felt the federal government was not doing enough to address the limited availability of COVID-19 testing. 58% felt the federal government was not doing enough to prevent a second wave of COVID-19 cases later in 2020.[243] In September 2020, the Pew Research Center found that the global image of the United States had suffered in many foreign nations. In some nations, the United States' favorability rating had reached a record low since Pew began collecting this data nearly twenty years earlier. Across thirteen different nations, a median of fifteen percent of respondents rated the U.S. response to the pandemic positively.[244]

The pandemic, along with the resultant stock market crash and other impacts, led a recession in the United States following the economic cycle peak in February 2020.[245] The economy contracted 4.8 percent from January through March 2020,[246] and the unemployment rate rose to 14.7 percent in April.[247] The total healthcare costs of treating the epidemic could be anywhere from $34 billion to $251 billion according to analysis presented by The New York Times.[248] A study by economists Austan Goolsbee and Chad Syverson indicated that most economic impact due to consumer behavior changes was prior to mandated lockdowns.[249] During the second quarter of 2020, the U.S. economy suffered its largest drop on record, with GDP falling at an annualized rate of 32.9 percent. As of June 2020, the U.S. economy was over ten percent smaller than it was in December 2019.[250]
.jpg/440px-President_Trump_and_the_Vice_President_meet_with_Airline_CEOs_about_the_Coronavirus_(49618513938).jpg)
In September, Bain & Company reported on the tumultuous changes in consumer behavior before and during the pandemic. Potentially permanently, they found acceleration towards e-commerce, online primary healthcare, livestreamed gym workouts, and moviegoing via subscription television. Concurrent searches for both low-cost and premium products, and a shift to safety over sustainability, occurred alongside rescinded bans and taxes on single-use plastics, and losses of three to seven years of gains in out-of-home foodservice.[251] OpenTable estimated in May that 25 percent of American restaurants would close their doors permanently.[252]
The economic impact and mass unemployment caused by the COVID-19 pandemic raised fears of a mass eviction crisis,[253][254][255][256] with an analysis by the Aspen Institute indicating 30–40 million are at risk for eviction by the end of 2020.[257][258][needs update] According to a report by Yelp, about sixty percent of U.S. businesses that have closed since the start of the pandemic will stay shut permanently.[259]
The pandemic has had far-reaching consequences beyond the disease itself and efforts to contain it, including political, cultural, and social implications.
From the earliest days of the pandemic, there were reported incidents of xenophobia and racism against Asian Americans.[36] During the first year, an ad-hoc organization called Stop AAPI Hate received 3,795 reports of racism against Asian Americans and Pacific Islanders.[267]
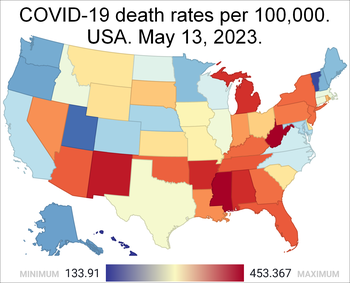
Disproportionate numbers of cases have been observed among Black and Latino populations.[30][31][32] Of four studies published in September 2020, three found clear disparities due to race and the fourth found slightly better survival rates for Hispanics and Blacks.[268] As of September 15, 2020, Blacks had COVID-19 mortality rates more than twice as high as the rate for Whites and Asians, who have the lowest rates.[269] CNN reported in May 2020 that the Navajo Nation had the highest rate of infection in the United States.[270] In June 2021, the CDC confirmed these numbers, reporting that American Indian or Alaska Native, Non-Hispanic persons had the highest rates of both hospitalizations and deaths, while Hispanic and Latino persons suffered the highest rates of COVID compared to White persons. However, the CDC noted that only 61% of case reports included race and ethnicity data, which could result in inaccurate estimates of the relative risk among groups.[271] Additionally, a study published by the New England Journal of Medicine in July 2020 revealed that the effect of stress and weathering on minority groups decreases their stamina against COVID.[272]
From 2019 to 2020, in the United States, the life expectancy of a Hispanic American decreased three years, for an African American 2.9 years, and for a White American 1.2 years.[45] The COVID Tracking Project[273] published data revealing that people of color were contracting and dying from COVID-19 at higher rates than Whites. An NPR analysis of April–September 2020 data from the COVID Tracking Project found that Black people's share of COVID-19 deaths across the United States was 1.5 times greater (in some states 2.5 times greater) than their share of the U.S. population. Similarly, Hispanics and Latinos were disproportionately infected in 45 states and had a disproportionate share of the deaths in 19 states. Native American and Alaskan Native cases and deaths were disproportionally high in at least 21 states and, in some, as much as five times more than average. White non-Hispanics died at a lower rate than their share of the population in 36 states and D.C.[274]
Life expectancy continued to fall from 2020 to 2021.[47][275]
By April 2020, closed schools affected more than 55 million students.[276] Higher education was also impacted in a variety of different ways.[277][278]
The pandemic prompted calls from voting rights groups and some Democratic Party leaders to expand mail-in voting, while Republican leaders generally opposed the change. Some states were unable to agree on changes, resulting in lawsuits. Responding to Democratic proposals for nationwide mail-in voting as part of a COVID-19 relief law, President Trump said "you'd never have a Republican elected in this country again" despite evidence the change would not favor any particular group.[279] Trump called mail-in voting "corrupt" and said voters should be required to show up in person, even though, as reporters pointed out, he had himself voted by mail in the last Florida primary.[280] Though mail-in vote fraud is slightly higher than in-person voter fraud, both instances are rare, and mail-in voting can be made more secure by disallowing third parties to collect ballots and providing free drop-off locations or prepaid postage.[281]
High COVID-19 fatalities at the state and county level correlated with a drop in expressed support for the election of Republicans, including the reelection of Trump, according to a study published in Science Advances that compared opinions in January–February 2020 with opinions in June 2020.[282]
The impact of the COVID-19 pandemic on hospitals became severe for some hospital systems of the United States in the spring of 2020, a few months after the COVID-19 pandemic began. Some had started to run out of beds, along with having shortages of nurses and doctors. By November 2020, with 13 million cases so far, hospitals throughout the country had been overwhelmed with record numbers of COVID-19 patients. Nursing students had to fill in on an emergency basis, and field hospitals were set up to handle the overflow.
At the beginning of 2021, cases had reached a peak, forcing some hospitals to periodically close their doors because they were overwhelmed with COVID-19 patients. In some places, as hospital space filled up, ambulances often waited hours to deliver patients. In addition, patients already admitted might get discharged earlier than usual to make room for others more severely ill. By early September, at least seven states had called in their National Guard to help overworked hospitals, including Oregon, Idaho, Montana, Kentucky, Tennessee, Georgia, and South Carolina.
The summer of 2021 saw another surge due to the new Delta variant of the virus. As a result, health care in U.S. hospitals was severely affected and led to crisis standards of care. Many hospitals were thereby unable to offer adequate medical care as a result of tight resources. For example, one hospital system in Oregon had to cancel or delay hundreds of surgeries as of mid-August. Hospitals also began seeing younger patients. And some experts found that the Delta variant was often more severe among younger age groups, whose vaccination rates were lower.
States like California saw over ten times more cases than they had just a few months earlier. By mid-August 2021, nearly all states experienced double-digit growth in COVID-19 hospitalizations. Some, like Washington, had a 34% increase of patients over a single week in September. At various medical centers, ICUs had reached capacity, forcing doctors to postpone routine surgeries. In addition, countless hospitals were also short of beds and nurses, making care and response times a lot slower. It meant that patients might wait in the ER for many hours. While some hospitals with no more capacity had to find alternate medical facilities in other states, often hundreds of miles away.
Emergency medical services in the United States also experienced a significant labor shortage, lengthening the time it took some patients to be transported to a hospital.The US map below is for the percent of people of all ages who received all doses prescribed by the initial COVID-19 vaccination protocol. Two of the three COVID-19 vaccines used in the U.S. require two shots to be fully vaccinated. The other vaccine requires only one shot. Booster doses are recommended too.[283][284]

The COVID-19 vaccination campaign in the United States is an ongoing mass immunization campaign for the COVID-19 pandemic in the United States. The Food and Drug Administration (FDA) first granted emergency use authorization to the Pfizer–BioNTech vaccine on December 10, 2020,[286] and mass vaccinations began four days later. The Moderna vaccine was granted emergency use authorization on December 17, 2020,[287] and the Janssen (Johnson & Johnson) vaccine was granted emergency use authorization on February 27, 2021.[288] By April 19, 2021, all U.S. states had opened vaccine eligibility to residents aged 16 and over.[289] On May 10, 2021, the FDA approved the Pfizer-BioNTech vaccine for adolescents aged 12 to 15.[290] On August 23, 2021, the FDA granted full approval to the Pfizer–BioNTech vaccine for individuals aged 16 and over.[291]
The U.S. government began the campaign under the presidency of Donald Trump with Operation Warp Speed, a public–private partnership to expedite the development and manufacturing of COVID-19 vaccines. Joe Biden became the new President of the United States on January 20, 2021. Biden had an immediate goal of administering 100 million vaccine doses within his first hundred days in office, and signed an executive order which increased supplies for vaccination.[292][293][294] This goal was met on March 19, 2021.[295] On March 25, 2021, he announced he would increase the goal to 200 million within his first 100 days in office.[296] This goal was reached on April 21, 2021.[297]
By July 4, 2021, 67% of the United States' adult population had received at least one dose, just short of a goal of 70%. This goal was met on August 2, 2021. While vaccines have helped significantly reduce the number of new COVID-19 infections nationwide, states with below-average vaccination rates began to see increasing numbers of cases credited to the highly infectious Delta variant by July 2021, which led to an increased push by organizations and companies to begin imposing de facto mandates for their employees be vaccinated for COVID-19.
On September 9, 2021, President Biden announced plans by the federal government to use executive orders and emergency temporary standards enforced by OSHA to mandate the vaccination of all federal branch employees, and require that all companies with more than 100 employees regularly test all employees who are not yet fully vaccinated for COVID-19.[298] On January 26, 2022, OSHA withdrew the vaccine mandate for companies with more than 100 employees due to a ruling from the Supreme Court of the United States that blocked the mandate.[299][300]
As of November 2022, according to The Commonwealth Fund, COVID-19 vaccination in the United States has prevented an additional 3.2 million deaths, an additional 18.5 million hospitalizations, and an additional 120 million infections from COVID-19. Vaccination has also prevented an additional $899.4 billion in healthcare costs.[301] According to a June 2022 study published in The Lancet, COVID-19 vaccination in the United States prevented an additional 1.9 million deaths from December 8, 2020, to December 8, 2021.[302][303] According to a July 2022 study published in JAMA Network Open, COVID-19 vaccination in the United States prevented an additional 235,000 deaths, an additional 1.6 million hospitalizations, and an additional 27 million infections from December 1, 2020, to September 30, 2021.[304]By August 2021, more than 800 colleges and universities, over 200 health care companies and dozens of states, local governments and school districts, had some type of vaccination requirements.[305] President Biden appealed to public organizations and private companies to require employees to be vaccinated, which companies are now legally allowed to do.[306]
Until August to September 2021, many companies were giving bonuses for getting vaccinated.[307] Nonetheless, nearly 2,000 private hospitals and health systems had previously issued vaccine mandates. Many companies outside health care did the same, such as United Airlines, Tyson Foods, and Walmart among them. Washington state had already required vaccines for all state employees and contractors.[307] With the new Delta variant spreading infections more quickly due to its higher transmissibility, companies including Facebook, Google, and Salesforce, have already issued employee vaccine mandates.[308]
According to a USA Today poll from August 2021, 68% supported a business's right to refuse service to unvaccinated customers, and 62% supported employer's right to mandate vaccinations to its employees. In the same poll, 72% also felt that mandating masks was "a matter of health and safety" and should not be considered an infringement of personal liberty.[309]


Evidence from vaccine use during the pandemic shows vaccination can reduce infection and is most effective at preventing severe COVID-19 symptoms and death, but is less good at preventing mild COVID-19. Efficacy wanes over time but can be maintained with boosters.[312] In 2021, the CDC reported that unvaccinated people were 10 times more likely to be hospitalized and 11 times more likely to die than fully vaccinated people.[313][314]
The CDC reported that vaccine effectiveness fell from 91% against Alpha to 66% against Delta.[315] One expert stated that "those who are infected following vaccination are still not getting sick and not dying like was happening before vaccination."[316] By late August 2021, the Delta variant accounted for 99 percent of U.S. cases and was found to double the risk of severe illness and hospitalization for those not yet vaccinated.[317]
In November 2021, a study by the ECDC estimated that 470,000 lives over the age of 60 had been saved since the start of the vaccination roll-out in the European region.[318]
On 10 December 2021, the UK Health Security Agency reported that early data indicated a 20- to 40-fold reduction in neutralizing activity for Omicron by sera from Pfizer 2-dose vaccinees relative to earlier strains. After a booster dose (usually with an mRNA vaccine),[319] vaccine effectiveness against symptomatic disease was at 70%–75%, and the effectiveness against severe disease was expected to be higher.[320]
According to early December 2021 CDC data, "unvaccinated adults were about 97 times more likely to die from COVID-19 than fully vaccinated people who had received boosters".[321]
A meta-analysis looking into COVID-19 vaccine differences in immunosuppressed individuals found that people with a weakened immune system are less able to produce neutralizing antibodies. For example, organ transplant recipients need three vaccines to achieve seroconversion.[322] A study on the serologic response to mRNA vaccines among patients with lymphoma, leukemia, and myeloma found that one-quarter of patients did not produce measurable antibodies, varying by cancer type.[323]
In February 2023, a systematic review in The Lancet said that the protection afforded by infection was comparable to that from vaccination, albeit with an increased risk of severe illness and death from the disease of an initial infection.[324]
A January 2024 study by the CDC found that staying up to date on the vaccines could reduce the risk of strokes, blood clots and heart attacks related to COVID-19 in people aged 65 years or older or with a condition that makes them more vulnerable to said conditions.[325][326]On February 17, 2022, Governor Gavin Newsom announced a formal shift toward endemic management of COVID-19 in California, saying "we are moving past the crisis phase into a phase where we will work to live with this virus".[327]
During his State of the Union Address on March 1, 2022, Biden stated that "because of the progress we've made, because of your resilience and the tools we have, tonight I can say we are moving forward safely, back to more normal routines." However, he also stated that the federal government would "never just accept living with COVID-19", explaining that it would "continue to combat the virus as we do other diseases." The White House released a new action plan the next day, which included plans to make COVID-19 antiviral medication available for free to high-risk patients at testing locations such as pharmacies and clinics, funding in support of vigilance and preparedness in the event of new surges and variants, preventing the closure of schools and businesses, and ensuring global vaccine distribution.[328][329]
On April 26, 2022, Fauci said that the United States is "out of the pandemic phase"[330] and the following day, stated that "we're really in a transitional phase...into hopefully a more controlled phase and endemicity", but further clarified that "the world is still in a pandemic...we are still experiencing a pandemic" and the United States could still see new waves of infection. Fauci's comments follow a report from the CDC indicating that the United States has a much higher level of collective immunity at this time, due to the Omicron variant.[331]
On May 16, 2022, Joseph Wendelken, a spokesman for the Rhode Island Department of Health stated that COVID-19 is now "an endemic disease" and said "we should expect moderate increases and decreases in our COVID-19 levels over the coming months".[332] In an interview with 60 Minutes aired on September 18, 2022, Joe Biden declared that the pandemic stage of COVID-19 was over in the United States.[333]
The United States has experienced pandemics and epidemics throughout its history, including the 1918 Spanish flu, the 1957 Asian flu, and the 1968 Hong Kong flu pandemics.[334][335][336] In the most recent pandemic prior to COVID-19, the 2009 swine flu pandemic took the lives of more than 12,000 Americans and hospitalized another 270,000 over the course of approximately a year.[334]
According to the Global Health Security Index, an American-British assessment which ranks the health security capabilities in 195 countries, the U.S. was the "most prepared" nation in 2020.[337][338]In September 2019, the Trump administration terminated United States Agency for International Development's PREDICT program, a $200 million epidemiological research program initiated in 2009 to provide early warning of pandemics abroad.[339][340] The program trained scientists in sixty foreign laboratories to detect and respond to viruses that have the potential to cause pandemics. One such laboratory was the Wuhan lab that first identified the virus that causes COVID-19. After revival in April 2020, the program was given two 6-month extensions to help fight COVID-19 in the U.S. and other countries.[341][342]
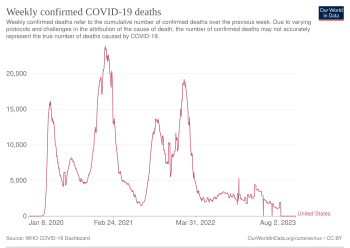
The CDC publishes official numbers of COVID-19 cases in the United States. The CDC estimates that, between February 2020 and September 2021, only 1 in 1.3 COVID-19 deaths were attributed to COVID-19.[343] The true COVID-19 death toll in the United States would therefore be higher than official reports, as modeled by a paper published in The Lancet Regional Health – Americas.[344] One way to estimate COVID-19 deaths that includes unconfirmed cases is to use the excess mortality, which is the overall number of deaths that exceed what would normally be expected.[345] From March 1, 2020, through the end of 2020, there were 522,368 excess deaths in the United States, or 22.9% more deaths than would have been expected in that time period.[346]
In February 2020, at the beginning of the pandemic, a shortage of tests made it impossible to confirm all possible COVID-19 cases[347] and resulting deaths, so the early numbers were likely undercounts.[348][349][350][351]Second Travel-related Case of 2019 Novel Coronavirus Detected in United States: The patient returned to the U.S. from Wuhan on January 13, 2020
'Foreign nationals other than immediate family of U.S. citizens and permanent residents who have traveled in China in the last 14 days will be denied entry into United States,' Azar said.
... effective February 2.
{{cite web}}: CS1 maint: multiple names: authors list (link)On Monday, April 10, 2023, the President signed into law: H.J.Res. 7, which terminates the national emergency related to the COVID-19 pandemic.
Data source: Centers for Disease Control and Prevention, Vaccine Breakthrough/Surveillance and Analytics Team.
Confirmed coronavirus cases in the U.S. crossed 200,000 on Thursday, but experts agree the actual number of infected people is much higher. The lack of reliable data—a persistent problem since the pandemic began—has made it impossible to determine the actual size of the outbreak, hampering the U.S. response.
Contributors: Danielle Allen • John M. Barry • John Bridgeland • Michael Callahan • Nicholas A. Christakis • Doug Criscitello • Charity Dean • Victor Dzau • Gary Edson • Ezekiel Emanuel • Ruth Faden • Baruch Fischhoff • Margaret "Peggy" Hamburg • Melissa Harvey • Richard Hatchett • David Heymann • Kendall Hoyt • Andrew Kilianski • James Lawler • Alexander J. Lazar • James Le Duc • Marc Lipsitch • Anup Malani • Monique K. Mansoura • Mark McClellan • Carter Mecher • Michael Osterholm • David A. Relman • Robert Rodriguez • Carl Schramm • Emily Silverman • Kristin Urquiza • Rajeev Venkayya • Philip Zelikow[1]
Dan Diamond; Charity Dean; Philip Zelikow;
Dan Diamond; Charity Dean ; Philip Zelikow ;
Dan Diamond; Charity Dean ; Philip Zelikow ;